Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(8):362-368
DOI 10.1590/S0100-72032012000800004
PURPOSE: To determine the nutritional status of vitamin E in breastfeeding women through the analysis of alpha-tocopherol concentration in serum and colostrum, to analyze its relation with maternal variables and to determine the prevalence of vitamin E deficiency in these women. METHODS: The study included 103 mothers who were classified according to maternal variables: age, nutritional status before pregnancy, gestational weight gain, parity and mode of delivery. Colostrum and serum samples were collected under fasting conditions in the immediate postpartum period. Alpha-tocopherol was analyzed by high performance liquid chromatography (HPLC). A serum cutoff of 697.7 μg/dL was adopted to define the nutritional status of vitamin E. Statistical analysis was performed with the Student's t test for independent samples and Pearson's correlation. Differences were significant when p<0.05. RESULTS: The average concentration of alpha-tocopherol was 1.125±551.0 μg/dL in colostrum and 1,138.6±346.0 μg/dL in serum, indicating adequate biochemical nutritional status. However, when analyzing the mothers individually, a 16% rate of subclinical vitamin E deficiency was detected. Women undergoing cesarean delivery had significantly higher alpha-tocopherol levels in colostrum (1.280±591 μg/dL) compared with those undergoing normal delivery (961.7±370 μg/dL) (p<0.05). It was found that mothers who were overweight before pregnancy had higher vitamin concentration in colostrum (1,331.5±548 μg/dL) when compared to underweight women (982.1±374 μg/dL) or women of normal weight (992.3±346 μg/dL) (p<0.05). However, the other variables were not associated with alpha-tocopherol in colostrum. Moreover, no variable showed association with vitamin E levels in maternal serum and no correlation was demonstrated between the alpha-tocopherol levels in serum and in milk. CONCLUSIONS: Despite the diagnosis of satisfactory nutritional status, breastfeeding women showed significant risk of subclinical vitamin E deficiency. We suggest that the concentration of alpha-tocopherol in colostrum be associated with type of delivery and pre-gestational nutritional status of women.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(8):363-367
DOI 10.1590/S0100-72032013000800005
PURPOSE: To evaluate the perinatal factors that influence the incidence of necrotizing enterocolitis (NEC) in newborns infants (NBI) weighing less than 1,500 g. METHODS: A prospective study that analyzed all infants with birth weight (BW) less than 1,500 g born between January 2006 to December 2010 (n=183). They were divided into two groups, i.e. infants diagnosed with NEC (n=18) and infants without a diagnosis of NEC (n=165), which were compared in terms of perinatal factors that could influence the incidence of NEC. Mean data were compared by Student's t-test or nonparametric tests and percentages of categorical variables were compared by the χ² test. When the variables showed differences between groups, they were analyzed using logistic regression with the dependent variable as the presence of NEC. The statistical package used was SPSS 16.0 for Windows. RESULTS: The two groups were similar in terms of most of the clinical and demographic neonatal and maternal data, except for the presence of preeclampsia (PE), which was higher in patients whose children developed NEC (61.1 versus 35,6%). The presence of PE increased the chance of occurrence of NEC by 2.84 times (95%CI 1.0 - 7.7). CONCLUSION: The only factor that can interfere with the incidence of NEC in infants of very low birth weight was the presence of PE. Awareness of this fact can guide the perinatal team in providing more judicious care regarding the prevention of NEC in this specific population.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(6):363-370
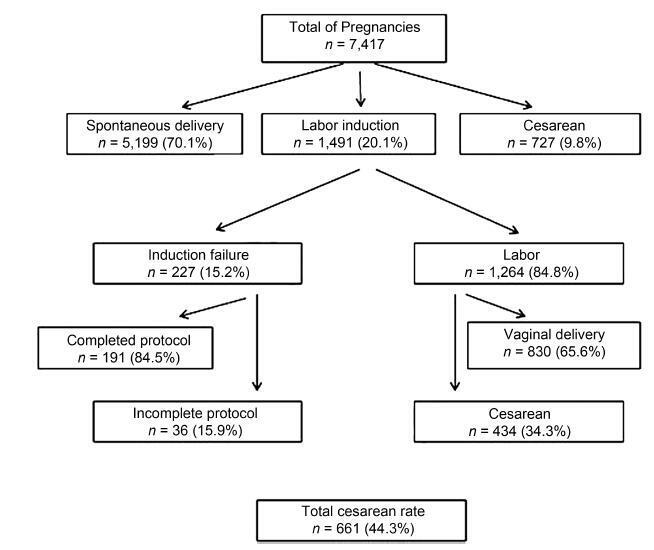
To evaluate the results of induced labor and to determine the main factors associated with intrapartum cesarean section after patients being submitted to this procedure at the Hospital Universitário of the Universidade Federal de Santa Catarina (HU/UFSC, in the Portuguese acronym), Florianópolis, state of Santa Catarina, Brazil.
A retrospective cross-sectional study that included all the pregnancies that resulted in single-fetus births, whose gestational-age was > 22 weeks and that had been submitted to labor induction at the HU/UFSC in the period from 2013 to 2016.
During the proposed period, 1,491 pregnant women were submitted to the labor induction protocol. In 1,264 cases (84.8%), induction resulted in labor, with 830 (65.7%) progressing to vaginal delivery. Gestational age ≥ 41 + 0 weekswas themost common indication for induced labor (55.2%), and vaginal administration of misoprostol was themost commonly usedmethod (72.0%). Among these pregnant women, the cesarean section rate was of 34.3%. Considering the cases of induction failure, the cesarean section rate rose to 44.3%. The factors associated with cesarean section were: previous history of cesarean delivery (PR [prevalence ratio] = 1.48; 95%CI [confidence interval]: 1.51-1.88), fetuses with intrauterine growth restriction (IUGR) (PR = 1.82; 95%CI: 1.32-2.19), Bishop score ≤ 6 (PR = 1.33; 95%CI: 1.01-1.82), and induction time either < 12 hours (PR = 1.44; 95%CI: 1.17-1.66) or > 36 hours (PR = 1.51; 95% CI 1.22-1.92) between the beginning of the induction and the birth.
Labor induction was successful inmost patients. In the cases in which the final outcome was a cesarean section, the most strongly associated factors were: previous history of cesarean delivery, presence of fetuses with IUGR, and either excessively short or excessively long periods of induction.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2010;32(8):363-367
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(5):363-367
DOI 10.1590/S0100-72032004000500004
OBJECTIVE: evaluation of fetomaternal hemorrhage (FMH) in patients who would need Rh alloimmunization with anti-D immunoglobulin (300 mug) prophylaxis after early miscarriage. METHOD: we included in the study Rh (D) negative blood group patients with positive or unknown Rh (D) partners, who had had a miscarriage up to 12 weeks of gestation, and had been admitted to hospital for uterine curettage. After this procedure 5 ml of venous blood was collected from the patients and the rosette test was applied to screen which patients would need quantitative determination of fetal blood transferred to the maternal circulation, by the Kleihauer-Betke test (K-B). RESULTS: out of 26 patients evaluated the rosette test was positive in one , who showed an FMH of 1.5 ml in the K-B test. CONCLUSIONS: the dose of anti-D immunoglobulin used in cases of miscarriage up to 12 weeks of gestation should be substantially reduced. The availability of preparations of 50 mug is recommended, for a more inexpensive and rational treatment.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(6):365-371
DOI 10.1590/S0100-72032000000600007
Purpose: to evaluate the accuracy of prenatal ultrasound in the diagnosis of nephrouropathies. Methods: the authors followed-up 127 pregnancies referred to the Fetal Medicine Center of UFMG with suspicion of these anomalies. Fetal biometry, growth, vitality, and associated malformations were evaluated. Finally, a detailed description of the renal system was made to define the prenatal morphologic diagnosis of the malformations to be compared with the postnatal diagnosis. Results: based on the kappa index (statistical method that measures the concordance between different measurements, methods or measurement instruments: below 0.40, poor agreement; between 0.40 and 0.75, good agreement; above 0.75, excellent ageement), the authors found an excellent concordance (kappa index 0.95). Among the 127 cases, there were only 9 misdiagnoses, all of them of obstructive uropathies: 6 cases showed different obstruction levels after delivery and in three cases there were confounding diagnosis with multicystic kidney. Conclusions: the detailed ultrasonographic description of the renal system is a good method for prenatal diagnosis of the fetal nephropathies, allowing some options to modify the outcome of these fetuses, like to send them to specialized centers, to anticipate delivery and even to apply intrauterine therapy, in order to preserve the renal function. Serial echography and amnioinfusion can be used to improve the precision of prenatal diagnosis.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2002;24(6):365-370
DOI 10.1590/S0100-72032002000600002
Purpose: to study the relationship between pelvic floor function and bladder neck mobility in women with and without stress urinary incontinence (SUI), in menacme and postmenopausal. Methods: sixty-one SUI patients were evaluated; 31 of them were in menacme and of these 17 had SUI and 14 did not have any complaint; 30 were postmenopausal and of these, 15 with SUI and 15 without SUI. Simple cystometry and empty supine stress test were performed in those who had urinary incontinence complaint. Bladder neck mobility was studied by ultrasound and by the Q-tip test. To study pelvic floor function, vaginal cones and digital palpation were used. Results: the bladder neck position in the incontinent women (Groups A and C), determined by ultrasound or the Q tip-test, was --11.8 cm in Group A and --12.5 cm in Group C, lower than the continent women, in whom the bladder neck was at +4.4 cm in Group B and +2.3 cm in Group D. There were no differences in bladder neck mobility among the continent menacme (9.1 cm) and postmenopausal (9.5 cm) groups. Also there were no differences among the incontinent groups (17.1 cm for Group A and 16.6 cm for Group C). The bladder neck mobility was greater in the incontinent women (A and C). Continent women had better results on evaluation of pelvic floor muscles than the incontinent ones, even using vaginal cones or digital palpation, and these results were not dependent on the hormonal status. Conclusion: a positive correlation was found between the Q-tip tests and ultrasound, and between test with vaginal cones and digital palpation. No significant correlation was found between pelvic floor function and bladder neck mobility.