Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(5):323-328
DOI 10.1590/S0100-72032003000500004
PURPOSE: to determine whether an elective cesarean section at the 38th week of gestation for HIV positive patients, in spite of decreasing vertical transmission, increases the risk of maternal death. METHODS: fifty-eight HIV-infected patients were studied and submitted to the complete ACTG 076 protocol (oral administration of zidovudine in the prenatal period associated with the intravenous form at delivery) followed by an elective cesarean section at the 38th week of gestation. The control group consisted of 226 noninfected women (the first four patients submitted to an elective cesarian section after each cesarian section in infected patient). The analyzed variables were: uterine atonia, puerperal fever, abdominal wall infection, urinary infection, endometritis, average blood loss, surgery time, and hospitalization time. Data were analyzed by the c² test (the Fisher test was used when there were less than 5 cases). The relative risk was calculated with the Epi-Info 6.0 program. RESULTS: results show that the elective cesarean section performed on HIV-positive patients, when compared to the control group, did not present a higher incidence of uterine atonia, puerperal fever, abdominal wall infection, urinary infection or endometritis. However, a greater average blood loss (2.26 relative risk) was recorded as well as an extended surgery time (3.32 relative risk). The HIV-infected patients remained less time in hospital than the noninfected control group (0.33 relative risk). CONCLUSION: we conclude that there was no increase in maternal morbidity after cesarean section as a means of interrupting gestation in the HIV-infected patients.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(6):324-328
DOI 10.1590/S0100-72032007000600008
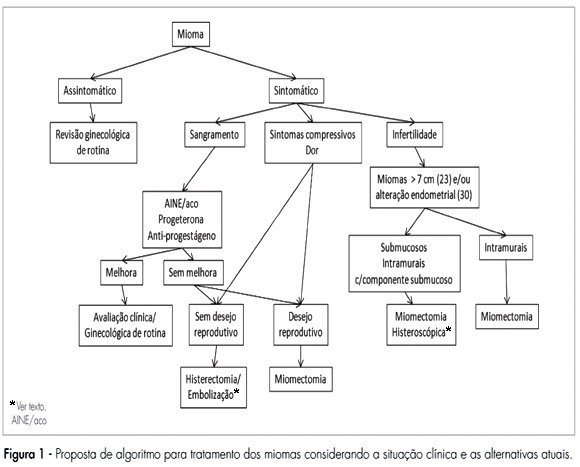
Leiomyomas are benign tumors. They appear in the myometrium and present a variable amount of fibrous conjunctive tissue. About 75% of the cases are not symptomatic and are usually found during abdominal, bimanual pelvic examination or during ultrasonography. The symptoms are directly related to the size, number and localization of the myomas. In the present review, the current clinical therapeutic procedures (oral anti-conceptive drugs, progestins and anti-progestins, analogues of the gonadothrophins’ releasing hormone (GnRH), and non-steroid anti-inflammatory drugs), and also the surgical procedures (hysterectomy, myomectomy, embolization) are presented for the treatment of leiomyomas.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(6):324-330
DOI 10.1590/S0100-72032006000600002
PURPOSE: to compare the maternal factors, clinical aspects and perinatal results in placental abruption during two periods. METHODS: retrospective analysis of placental abruption cases that occurred from January 1, 1994 through December 31, 1997 (period 94-97), and from April 4, 2001 through March 3, 2005 (period 01-05), in singleton delivery with birthweight higher than 500 g and after 20 weeks of gestation. The following factors were analyzed: maternal age, previous obstetric history, prenatal care, premature rupture of membranes, obstetric and/or clinical intercurrent events, vaginal bleeding, uterine tonus, fetal anomaly, mode of delivery, hemoamnion and maternal complication (hysterectomy, uterine atony, disseminated intravascular coagulation, acute renal failure, and maternal death), and the perinatal results. RESULTS: the rate of placental abruption was 0.78% (60 cases) in the period 94-97 (n=7692 deliveries), and 0.59% (51 cases) in the period 01-05 (n=8644 deliveries), without significant difference. A significant difference was observed between the periods 94-97 and 01-05 regarding mean number of previous gestations (3.5±2.4 and 2.6±1.8, p=0.04), patients without prenatal care (13.3 and 2.0%, p=0.03) and maternal intercurrences (38.3 and 64.7%, p=0.01). No significant difference was observed related to vaginal bleeding, tonus abnormalities and perinatal results, between the periods, but a higher proportion of hemoamnion in 94-97 was found when compared to 01-05 (28.3 and 11.8%, p=0.03). CONCLUSIONS: in spite of obstetrical advances, maternal complications and perinatal results were similar in the analyzed periods. The severity and the unexpected results emphasize the importance of prevention and adequate control of associated factors, when this pathology is approached.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2016;38(7):325-332
Systematic reviews that evaluate the perineal cryotherapy to reduce pain in the vaginal postpartum are inconclusive.
To evaluate clinical effectiveness of cryotherapy in the management of humanized postpartum perineal pain and vaginal edema.
A double-bind randomized controlled clinical trial (UTN number: U1111- 1131-8433) was conducted in a hospital in Northeastern, Brazil.Women were included following humanized childbirth. All had vaginal deliveries of a single, full-term pregnancy with cephalic presentation. Exclusion criteria included previous perineal lesion, episiotomy during the current delivery, instrumental delivery, uterine curettage and postpartum hemorrhage. In the experimental group, an ice pack was applied six times on the perineum for 20 minutes, reducing the temperature between 10 and 15° C, then 60 minutes without exposure to cold. In the non-cryotherapy, a water bag unable to reduce the temperature to this extent was used, compliance with the same application protocol of the first group. Perineal temperature wasmonitored at zero, 10 and 20 minutes for application in both groups. Evaluations were made immediately before and after the applications and 24 hours after delivery spontaneous, to determine the association between variables.
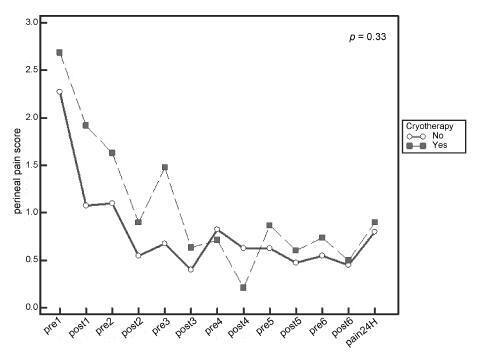
A total of 80 women were included in the study, 40 in each group. There was no significant difference in scores of perineal pain and edema between the groups with or without cryotherapy until 24 hours after childbirth. There was no difference between groups when accomplished repeated measures analysis over the 24 hours after delivery, considering the median perineal pain (p = 0.3) and edema (p = 0.9). Perineal cryotherapy did not influence the amount of analgesics used (p = 0.07) and no adverse effect was registered.
The use of cryotherapy following normal vaginal delivery within the concept of humanized minimally interventionist childbirth had no effect on perineal pain and edema, since it was already substantially lower, nor the need for pain medicaments.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2015;37(7):325-332
DOI 10.1590/S0100-720320150005367
To determine the eating behavior of pregnant women assisted by primary health care and to compare it with women at childbearing age in Brazilian capitals.
A cross-sectional study conducted on 256 pregnant women in the second trimester of gestation, selected by drawing lots from those assisted by primary health care units of a municipality in the state of São Paulo in 2009/2010. Eating habits were investigated via a questionnaire adapted from the VIGITEL system, consisting of questions about eating habits in general and the frequency and consumption characteristics of food groups/specific foods. For tis comparison, we used the indicators reported by the VIGITEL system for women at childbearing age in Brazilian capitals in 2010. The analyses involved the presentation of frequency distribution and descriptive statistics with comparisons according to the age group.
Most patients had breakfast every day (86.7%) and 45.7% habitually exchanged a main meal for a snack once or twice a week. A daily consumption of fruit, raw salad and vegetables was not reported by 48.8%, 41.8% and 55.1% of the women, respectively. Fish was reported to never or almost never be consumed by 64.4% of the pregnant women. At least once a week, 69.9% of them reported the consumption of soda, and 86.4% of wafers/cookies. The comparison between the pregnant women and women at childbearing age in capitals showed a close similar prevalence of overweight, and no difference in the regular consumption of fruit and vegetables. Meat containing excess of fat and whole milk were more consumed by pregnant women, with differences reported in all the age groups analyzed. On the other hand, the pregnant women reported a less regular intake of soft drinks.
The actions that need to be performed in prenatal care are various and very important, promoting the consumption of specific foods and providing guidelines about eating behavior, while reinforcing healthy eating habits already present.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(7):325-327
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(6):325-331
DOI 10.1590/S0100-72032000000600002
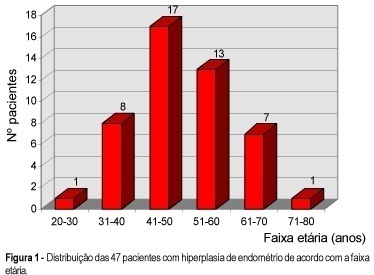
Purpose: to evaluate the efficacy of medroxyprogesterone acetate and megestrol acetate in endometrial hyperplasia. Patients and Methods: forty-seven patients with abnormal uterine bleeding were retrospectively evaluated. These patients were submitted to diagnostic uterine curettage and/or endometrial biopsy, with histopathological finding of endometrial hyperplasia. Patients with hyperplasia without atypia received 10 mg/day oral medroxyprogesterone acetate during 10 to 12 days a month. Those with hyperplasia with atypia received 160 mg/day oral megestrol acetate continuously. The length of treatment ranged from 3 to 18 months. Control endometrial biopsy and/or uterine curettage were performed 3 and 6 months from the beginning of treatment, and then periodically to evaluate whether or not regression of hyperplasia occurred. Results: forty-two patients with endometrial hyperplasia without atypia and 5 with hyperplasia with atypia were included. The mean age of the patients was 49.5 ± 10.6 years (22 to 72 years), 70.2% aged over 45 years. Medroxy-progesterone acetate was effective in promoting regression of 83.2% (35/42) of hyperplasia without atypia, and megestrol acetate in 80% (4/5) of hyperplasia with atypia. Despite treatment, lesions persisted in 16.8% (7 cases) of hyperplasia with atypia and in 20% (1 case) of hyperplasia without atypia. No progression to endometrial cancer was seen during the follow-up period of 3 months to 9 years. During follow-up, we found that 18 patients (38.3%) showed amenorrhea, 12 (25.5%) menstrual cycle regulation, and 17 (36.2%) persistent abnormal uterine bleeding and underwent total abdominal hysterectomy. Histological examination of the uterus showed 8 patients with persistence of hyperplastic lesion, 4 with leiomyoma, 3 with adenomyosis, 1 with diffuse uterine myohypertrophy, and 1 with normal uterus, despite regression of the hyperplastic lesions in 9 of the 17 patients. Conclusions: the treatment of endometrial hyperplasia with medroxyprogesterone acetate and megestrol acetate can be a safe alternative for women who refuse to have their uterus removed or those at high risk for surgery. However, a careful monitoring of the endometrium is needed. This can be achieved with periodical endometrial biopsy, transvaginal ultrasonography, and evaluation of the symptoms.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(6):325-332
To evaluate the insertion of the hysteroscopic intratubal sterilization device for female sterilization concerning the technique and the feasibility.
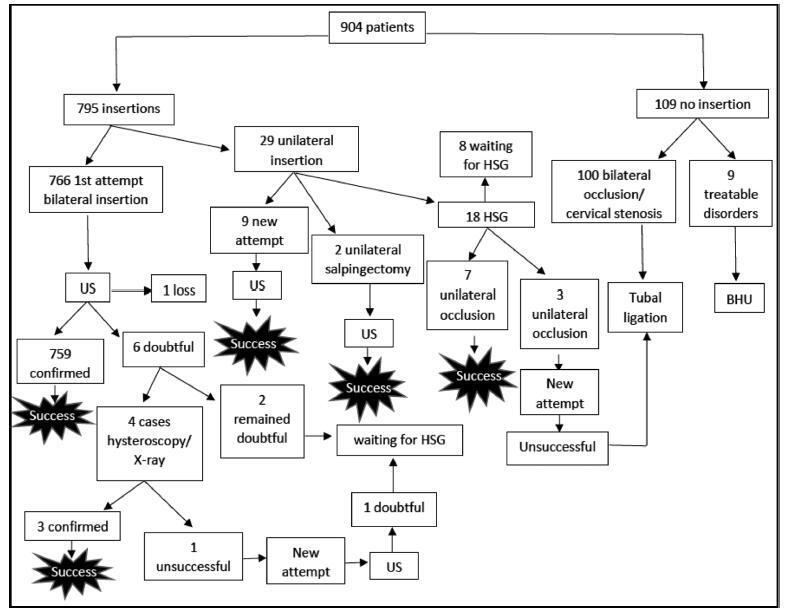
Retrospective study with data collection of medical records of 904 patients who underwent device insertion between January and September 2016 in a public hospital in Rio de Janeiro (Brazil) with data analysis and descriptive statistics.
In 85.8% of the cases, the uterine cavity was normal, and themost commonlydescribed findings upon hysteroscopy were synechiae (9.5%). The procedure lasted an average of 3.56minutes (range: 1 to 10minutes), and the pain was considered inexistent or mild in 58,6% of the cases, mild or moderate in 32,8%, and severe or agonizing in less than 1% (0.8%) of the cases, based on a verbal scale ranging from 0 to 10. The rate of successful insertions was of 85.0%, and successful tubal placement was achieved in 99.5% of the cases. There were no severe complications related to the procedure, but transient vasovagal reactions occurred in 5 women (0.6%).
Female sterilization performed by hysteroscopy is a safe, feasible, fast, and well-tolerated procedure. The rates of successful insertions and tubal placements were high. There were few and mild adverse effects during the procedure, and there were no severe complications on the short term.