Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2002;24(5):309-313
DOI 10.1590/S0100-72032002000500004
Purpose: to evaluate the importance of endometrial thickness measurement as an orienting factor for the clinical treatment of unruptured tubal pregnancy. Method: longitudinal observational study, in which the greatest measure of the endometrial thickness was evaluated in millimeters, in the uterine longitudinal axis, through transvaginal ultrasonography. Our study group included 181 patients, all of them respecting the utilization criteria for the clinical treatment (expectant or medicated with methotrexate). Through Student's t test we evaluated the difference between the average thickness of the cases who presented successful results with the treatment and the average of those who failed. Results: the average endometrial thickness of the patients who presented successful results with the medical treatment (31 cases) was 6.4 mm, while the average in the cases of failure was 11.5 mm. These results were significantly different. The average thickness of the successful group with expectant management (128 cases) was 9.0 mm, while the average of those who failed was 9.6 mm. These values were not statistically different. Conclusions: the greatest measure of the endometrial thickness of the uterine longitudinal axis through transvaginal ultrasonography proved to be valuable as a new orienting factor for the medical treatment of patients with a diagnosis of unruptured tubal pregnancy. It may become a useful and auxiliary tool for the recommendation of the use of methotrexate. On the other hand, thickness did not show to be useful as an orienting factor for establishing expectant management.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(6):309-312
To study the structure ofmaternalmortality caused by abortion in the Tula region.
The medical records of deceased pregnant women, childbirth, and postpartum from January 01, 2001, to December 31, 2015, were analyzed.
Overall, 204,095 abortion cases were recorded in the Tula region for over 15 years. The frequency of abortion was reduced 4-fold, with 18,200 in 2001 to 4,538 in 2015. The rate of abortions per 1,000 women (age 15-44 years) for 15 years decreased by 40.5%, that is, from 46.53 (2001) to 18.84 (2015), and that of abortions per 100 live births and stillbirths was 29.5%, that is, from 161.7 (2001) to 41.5 (2015). Five women died from abortion complications that began outside of the hospital, which accounted for 0.01% of the total number. In the structure of causes of maternal mortality for 15 years, abortion represented 14.3% of the cases. Lethality mainly occurred in the period from 2001 to 2005 (4 cases). Among thematernal deaths, many women died in rural areas after pregnancy termination at 18 to 20 weeks of gestation (n = 4). In addition, three women died from sepsis and two from bleeding.
The introduction of modern, effective technologies of family planning has reduced maternal mortality due to abortion.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(6):309-314
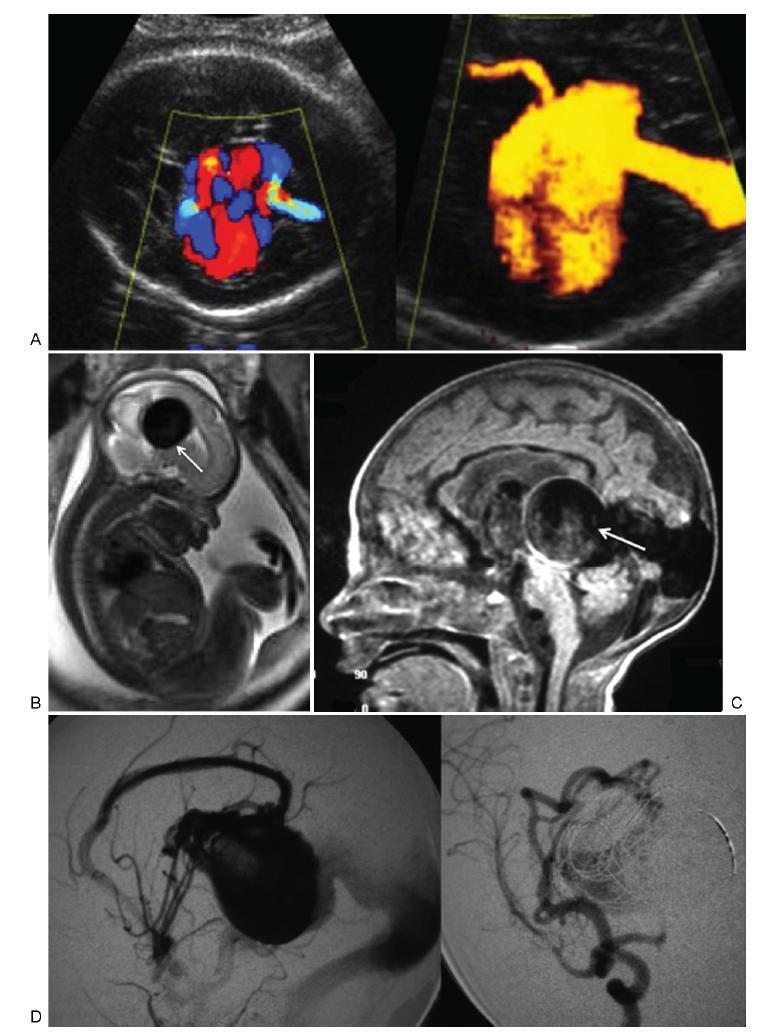
To describe the prenatal diagnosis of Galen vein aneurysm (GVA) based on ultrasonography and magnetic resonance imaging (MRI) in a series of cases, as well as its postnatal outcomes and follow-up until 4 years of age.
A retrospective longitudinal study was performed, analyzing a database comprising seven cases of prenatal diagnosis of GVA at two Brazilian institutions from February of 2000 to May of 2012. The following data were evaluated: gestational age at diagnosis, GVA dimensions on ultrasonography, associated fetal changes, findings on fetal echocardiography, gestational age at delivery, type of delivery, birth weight, Apgar score at the 1st and 5th minutes, neonatal outcomes, and survival with follow-up until 4 years of age.
The mean gestational age ± standard deviation on the prenatal diagnosis of GVA based on ultrasonography was 25±4.9 weeks. The mean length of GVA was 3.2±0.4 cm. The mean gestational age at birth was 37.5±0.7 weeks, and a cesarean section was performed in 85.7% of the cases (6/7). The mean birth weight was 3,070±240.4 g. The total survival rate was 42.8% (4/7), with three neonatal deaths. Of the four survivors, three presented with normal neuropsychomotor development until 4 years of age and only one showed serious neurological sequelae. Ultrasonography and MRI showed similar findings for all seven cases.
Galen Vein Aneurysm is associated with a high neonatal death rate. Therefore, its prenatal diagnosis is essential for parent counseling and follow-up at tertiary care institutions.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(5):309-316
DOI 10.1590/S0100-72032003000500002
PURPOSE: to determine the prevalence of domestic physical violence among women who delivered at a tertiary center in the Northeast of Brazil, to study the main risk factors associated with domestic violence, and to determine perinatal outcome. METHODS: a cross-sectional study was conducted, enrolling 420 women who delivered at a tertiary center in Recife (Brazil) with fetuses weighing more than 500 g. They were submitted to interviews with open and closed questions. The prevalence of domestic physical violence was determined. Statistical analysis was performed using c² and Fisher's exact tests at a 5% level of significance. The prevalence ratio was determined as measurement of relative risk of violence. Multiple logistic regression analysis was performed and the adjusted risk was calculated. RESULTS: the prevalence of domestic physical violence was 13.1% (95% CI = 10.1-16.6) and 7.4% (95% CI = 5.2-10.2) before and during pregnancy, respectively. The pattern of violence has changed during pregnancy: stopped in 43.6%, was reduced in 27.3% and increased in 11% of the victims. After multivariate analysis the variables that persisted strongly associated with violence were low female educational level, history of violence in the women´s family, partner's use of alcohol and unemployment. Perinatal outcome was studied and a significantly higher frequency of neonatal death was observed among victims of domestic violence. CONCLUSIONS: a high prevalence of domestic physical violence was observed (about 13%) in women who delivered at a tertiary center in Northeast of Brazil. The main risk factors were low educational level and previous familiar history of violence in the women's family, alcohol use by and unemployment of their partners. Neonatal mortality was increased in victims of violence.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(1):31-34
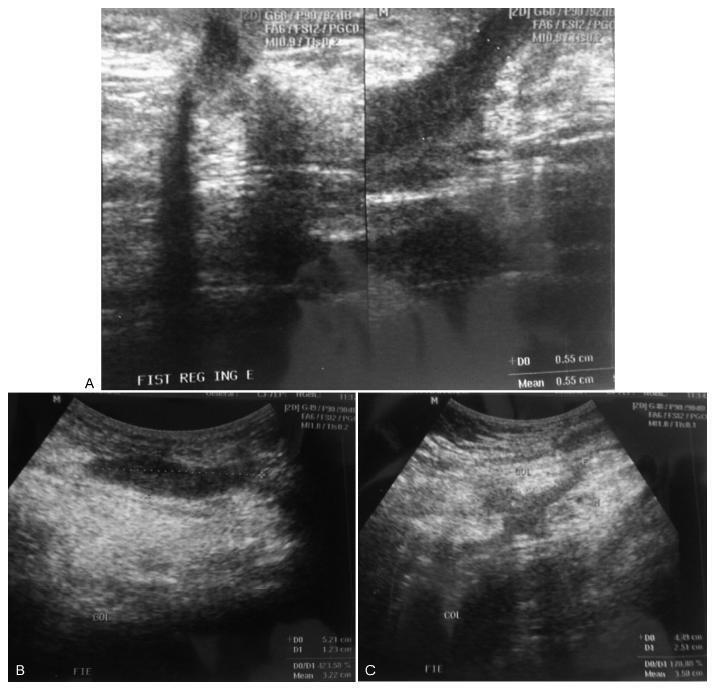
The development of a tubocutaneous fistula due to endometriosis in a post-cesarean section surgical scar is a rare complication that generates significant morbidity in the affected women. Surgery is the treatment of choice in these cases. Hormonal therapies may lead to an improvement in symptoms, but do not eradicate such lesions. In this report, we present a 34-year-old patient with a cutaneous fistula in the left iliac fossa with cyclic secretion. Anamnesis, a physical examination, and supplementary tests led us to suggest endometriosis as the main diagnosis, which was confirmed after surgical intervention.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2001;23(1):31-37
DOI 10.1590/S0100-72032001000100005
Purpose: to evaluate the prognosis of fetal omphalocele after prenatal diagnosis. Methods: fifty-one cases with prenatal diagnosis of fetal omphalocele were divided into three groups: group 1, isolated omphalocele; group 2, omphalocele associated with structural abnormalities and normal karyotype; group 3, omphalocele with abnormal karyotype. The data were analyzed for overall survival rate and postsurgery survival, considering associated malformations, gestational age at delivery, birth weight and size of omphalocele. Results: group 1 corresponded to 21% (n = 11), group 2, 55% (n = 28) and group 3,24% (n = 12). All of Group 3 died, and trisomy 18 was the most frequent chromosomal abnormality. The survival rate was 80% for group 1 and 25% for group 2. Sixteen cases underwent surgery (10 isolated and 6 associated), 81% survived (8 isolated and 5 associated). The median birth weight was 3,140 g and 2,000 g for survivals and non-survivals after surgery, respectively (p = 0.148), and the corresponding gestational age at delivery was 37 and 36 weeks (p = 0.836). The ratio of omphalocele/abdominal circumference decreased with gestation, 0.88 between 25-29 weeks and 0.65 between 30-35 weeks (p = 0.043). The size of omphalocele was not significantly different between the 3 groups (p = 0.988), and it was not associated to postsurgery prognosis (p = 0.553). Conclusion: the overall and postsurgery survival rates were 25 and 81%, respectively. Associated malformations were the main prognostic factor in prenatally diagnosed omphaloceles, since they are associated with prematurity and low birth weight.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(1):31-37
To evaluate the expulsion and continuation rates of the copper intrauterine device (IUD) inserted in the immediate postpartum period in a Brazilian public university hospital.
In the present cohort study, we included women who received immediate postpartum IUD at vaginal delivery or cesarean s March 2018 to December 2019. Clinical data and the findings of transvaginal ultrasound (US) scans performed 6-weeks postpartum were collected. The expulsion and continuation rates were assessed 6-months postpartum using data from the electronic medical records or by telephone contact. The primary outcome was the proportion of IUDs expelled at 6 months. For the statistical analysis, we used the Student t-test, the Poisson distribution, and the Chi-squared test.
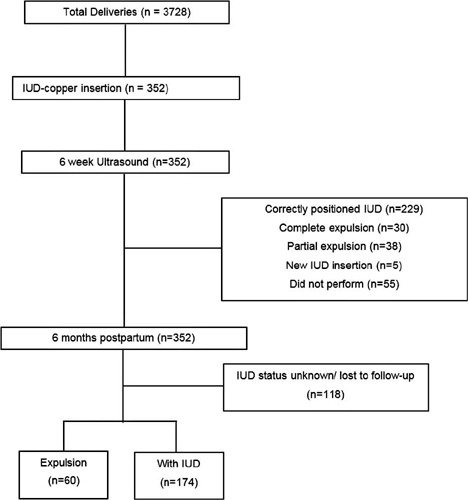
There were 3,728 births in the period, and 352 IUD insertions were performed, totaling a rate of 9.4%. At 6 weeks postpartum, the IUD was properly positioned in 65.1% of the cases, in 10.8% there was partial expulsion, and in 8.5% it had been completely expelled. At 6 months postpartum, information was obtained from 234 women, 74.4% of whom used IUD, with an overall expulsion rate of 25.6%. The expulsion rate was higher after vaginal delivery when compared with cesarean section (68.4% versus 31.6% respectively; p = 0.031). There were no differences in terms of age, parity, gestational age, final body mass index, and newborn weight.
Despite the low insertion rate of copper IUDs in the postpartum period and a higher expulsion rate, the rate of long-term continuation of intrauterine contraception was high, indicating that it is a useful intervention to prevent unwanted pregnancies and to reduce short-interval birth.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(1):31-35
DOI 10.1590/S0100-72032008000100006
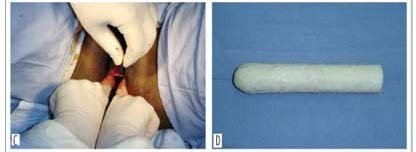
PURPOSE: to evaluate the use of natural latex mold (Hevea brasiliensis) as a modification of McIndoe and Bannister neovaginoplasty in patients presenting Mayer-Rokitansky-Küster-Hauser (MKRH) syndrome. METHODS: we retrospectively included nine patients presenting MKRH syndrome, who had been submitted to McIndoe and Bannister neovaginoplasty modified by the use of natural latex mold. Neovaginal epithelization and depth, coitus occurrence and satisfaction, and surgical complications were evaluated. RESULTS: five weeks after the procedure, eight patients presented an epithelized 7 to 12 cm deep neovagina. There was one case of complete neovaginal stenosis, because of incorrect use of the mold. After at least one year, the others maintained 4 to 8 cm deep neovaginas and capacity for intercourse, with 66.7% satisfaction. One woman presented precocious rectovaginal fistula and late episodes of uretrovaginal fistulae. Two patients presented distal neovaginal stenosis in long-term follow-up. One of these and the patient with fistulae were submitted to a new procedure. CONCLUSIONS: the use of natural latex mold as a modification of classic neovaginoplasty technique allows the creation of neovaginas morphologically and functionally similar to the normal vagina in patients with vaginal agenesis.