Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(5):294-295
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(5):294-294
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(6):294-299
DOI 10.1590/S0100-72032008000600005
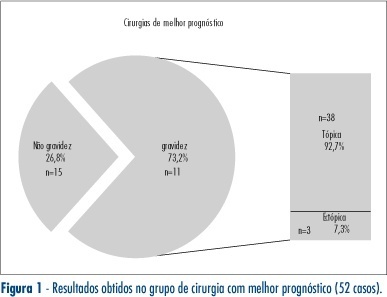
PURPOSE: to verify the ratio of intra-uterine gestation in patients submitted to recanalization in the Hospital Regional da Asa Sul in the last 30 years and to assess the rate of ectopic gestation of such procedures, the influence of age and time interval between salpingectomy and recanalization in the therapeutic success. METHODS: medical files of 71 patients were analyzed, after exclusion of those presenting other alterations that could influence fertility prognosis, plus the cases when recanalization was impossible. Variables collected were: occurrence of intra-uterine gestation, coming to term or to abortion; occurrence of ectopic pregnancy after salpingectomy; no-conception after reversion, women's age at the recanalization, and time interval between salpingectomy and its reversion. RESULTS: there has been a pregnancy rate of 67.6%, 73.2% for bilateral recanalization and 46.6% for unilateral, as well as 5.6% of ectopic pregnancies. Concerning the patients' age group, it was observed a pregnancy rate of 33%, from 20 to 24; 60%, from 25 to 29; 69.2%, from 30 to 34; 65%, from 35 to 39, and 42.9%, from 40 to 44 years old. The number of cases was small for age the groups 20 to 24 and 40 to 44 years old. The time interval between salpingectomy and recanalization (TISR) has varied from one to 18 years. TISR has been divided in three groups presenting the following pregnancy rates: one to six year interval, 59%; seven to 12, 66.6%; 13 to 18, 57%. CONCLUSIONS: gestation rate has been 67.6%, 5.6% being ectopic. In the comparison of age groups, there has been no significant influence of age on the therapeutic success of patients from 25 to 39 years old. Sterility duration did not influence the reversion results.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(5):294-299
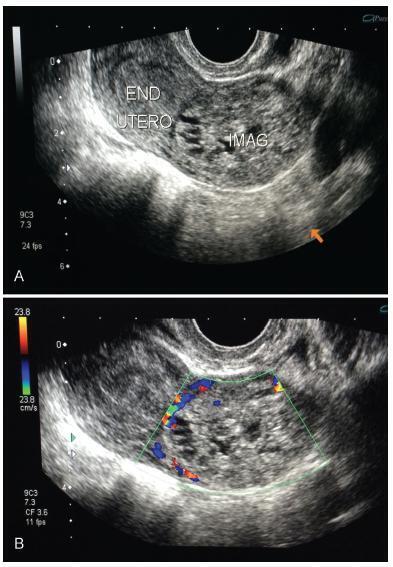
This report presents the case of a patient with gestational trophoblastic neoplasia after a partial hydatidiform mole formed in the Fallopian tube. Ectopic molar pregnancy is a rare condition, with an estimated incidence of 1 in every 20,000 to 100,000 pregnancies; less than 300 cases of it have been reported in the Western literature. The present report is important because it presents current diagnostic criteria for this rare condition, which has been incorrectly diagnosed in the past, not only morphologically but also immunohistochemically. It also draws the attention of obstetricians to the occurrence of ectopic molar pregnancy, which tends to progress to Fallopian tube rupture more often than in cases of ectopic non-molar pregnancy. Progression to gestational trophoblastic neoplasia ensures that patients with ectopic molar pregnancy must undergo postmolar monitoring, which must be just as thorough as that of patients with intrauterine hydatidiform moles, even if chemotherapy results in high cure rates.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(6):294-308
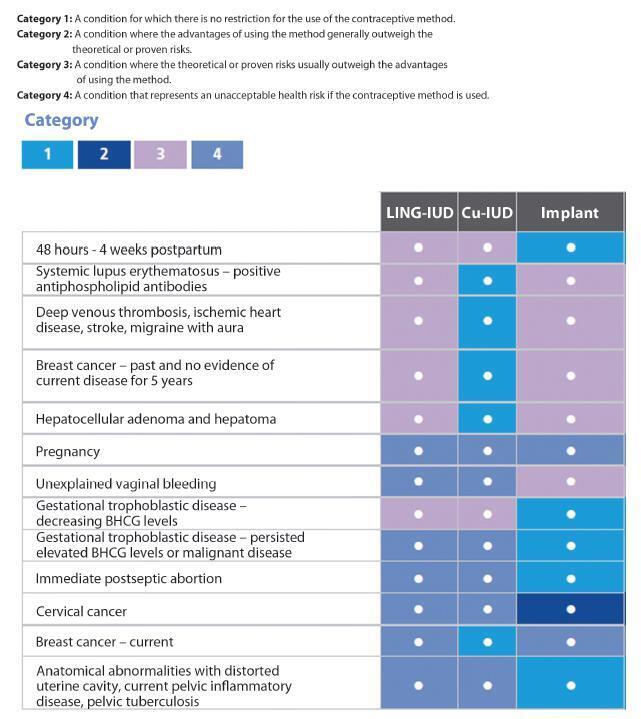
Unwanted pregnancy is a major public health problem both in developed and developing countries. Although the reduction in the rates of these pregnancies requires multifactorial approaches, increasing access to long-acting contraceptive methods can contribute significantly to change this scenario. In Brazil, gynecologists and obstetricians play a key role in contraceptive counseling, being decisive in the choice of long-acting reversible methods, characterized by intrauterine devices (IUDs) and the contraceptive implant. The vast scope due to the reduced number of situations to indicate long-acting methods should be emphasized in routine contraceptive counseling. On the other hand, gynecologists and obstetricians should adapt the techniques of insertion of long-acting methods, and engage in facilitating conditions to access these contraceptives through public and private health systems in Brazil. This study is part of a project called Diretrizes e Recomendações FEBRASGO (Guidelines and Recommendations of the FEBRASGO - Brazilian Federation of Gynecology and Obstetrics Associations from the Portuguese acronym). It aims to review the main characteristics of long-acting contraceptives and critically consider the current situation and future prospects to improve access to these methods, proposing practical recommendations of interest in the routine of gynecologists and obstetricians.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(7):295-300
DOI 10.1590/S0100-72032013000700003
PURPOSE: To evaluate the prevalence of women aged 50 years or more who are sexually active and their self-perception with respect to their sexual lives. Associated factors were also assessed. METHODS: A cross-sectional, population-based, self-reported household survey involving 622 Brazilian women aged 50 years or more. Sociodemographic, clinical, and behavioral factors were evaluated. The sexual life self-perception was classified as very good, good, fair, poor, or very poor. Data were analyzed using the χ² test, Fisher's exact test, and Poisson multiple regression analysis. Prevalence ratios and their 95% confidence intervals were also calculated. RESULTS: Of the women in this sample, 228 (36.7%) reported having a sexual life and, of these, 53.5% classified it as very good or good, while 46.5% considered it fair, poor, or very poor. The bivariate analysis indicated that being postmenopausal (p=0.025) and using natural remedies to treat the menopause (p=0.035) were factors associated with the woman classifying their sexual lives as fair, poor, or very poor. Multiple regression analysis showed that more women who had used or were currently using natural remedies for the menopause scored their sexual lives as fair, poor, or very poor. CONCLUSIONS: More than half the women aged 50 years or more in this study were not sexually active. A poorer sexual life self-perception was associated with the use of natural remedies to treat menopausal symptoms. This may indicate a need to improve the way in which these women are evaluated and treated. Women's assessment of their own sexual lives may prove a useful tool in clinical practice.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(4):295-298
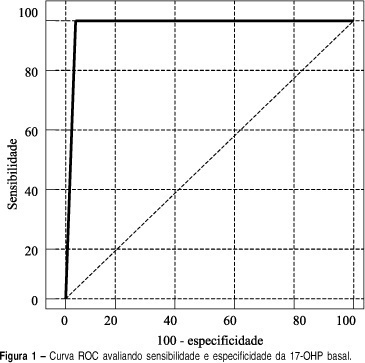
DOI 10.1590/S0100-72032004000400005
INTRODUCTION: adrenal hyperplasia is a common genetic disorder and 95% of the cases are due to a 21-hydroxylase deficiency. Clinical presentation varies from life-threatening salt-losing adrenal hyperplasia to simple androgenic states, which can be of late-onset and very similar to polycystic ovary syndrome. Diagnosis is usually made by synthetic ACTH provocative tests but efforts are being made to simplify this investigation. OBJECTIVE: to evaluate basal 17-hydroxyprogesterone as a predictor of the provocative test for the diagnosis of late-onset congenial adrenal hyperplasia. METHODS: A total of 122 patients under clinical suspicion of diagnosis of late-onset congenial adrenal hyperplasia were included and retrospectively evaluated in the study. Such suspicion included signs and/or symptoms of hyperandrogenism (hirsutism, acne, oily skin, menstrual irregularity etc.). All the patients were submitted to the 0.25mg synthetic ACTH provocative test (Synacthen®). After resting for 60 minutes, the samples were taken in the basal time and 60 minutes after the administration of 0.25mg synthetic ACTH, in order to assay 17-hydroxiprogesteron, the venous access being kept through a heparinized catheter. Radioimmuoessay was the method used to accomplish the assay of seric 17-hydroxiprogesteron. The sensitivity and specificity of the basal 17-hydroxiprogesteron were measured, assessing several cutoff points. ROC curves were made to analyze the test performance, using the software Medcalc®. RESULTS: ROC curve analysis showed that the best cutoff point was 181 ng/dl, which was very similar to the most common recommendation of 200 ng/dl of the literature. The cutoff point of 200 ng/dl shows positive and negative predictive values of 75 and 100%, and accuracy of 98,4% as a diagnostic test for late-onset adrenal hyperplasia. CONCLUSIONS: considering our data, we suggest that all hyperandrogenic patients should start the investigation with basal 17-hydroxyprogesteron and in case it is above 181 ng/dl, then they should do the synthetic 17-hydroxyprogesteron provocative test.