Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-FPS02
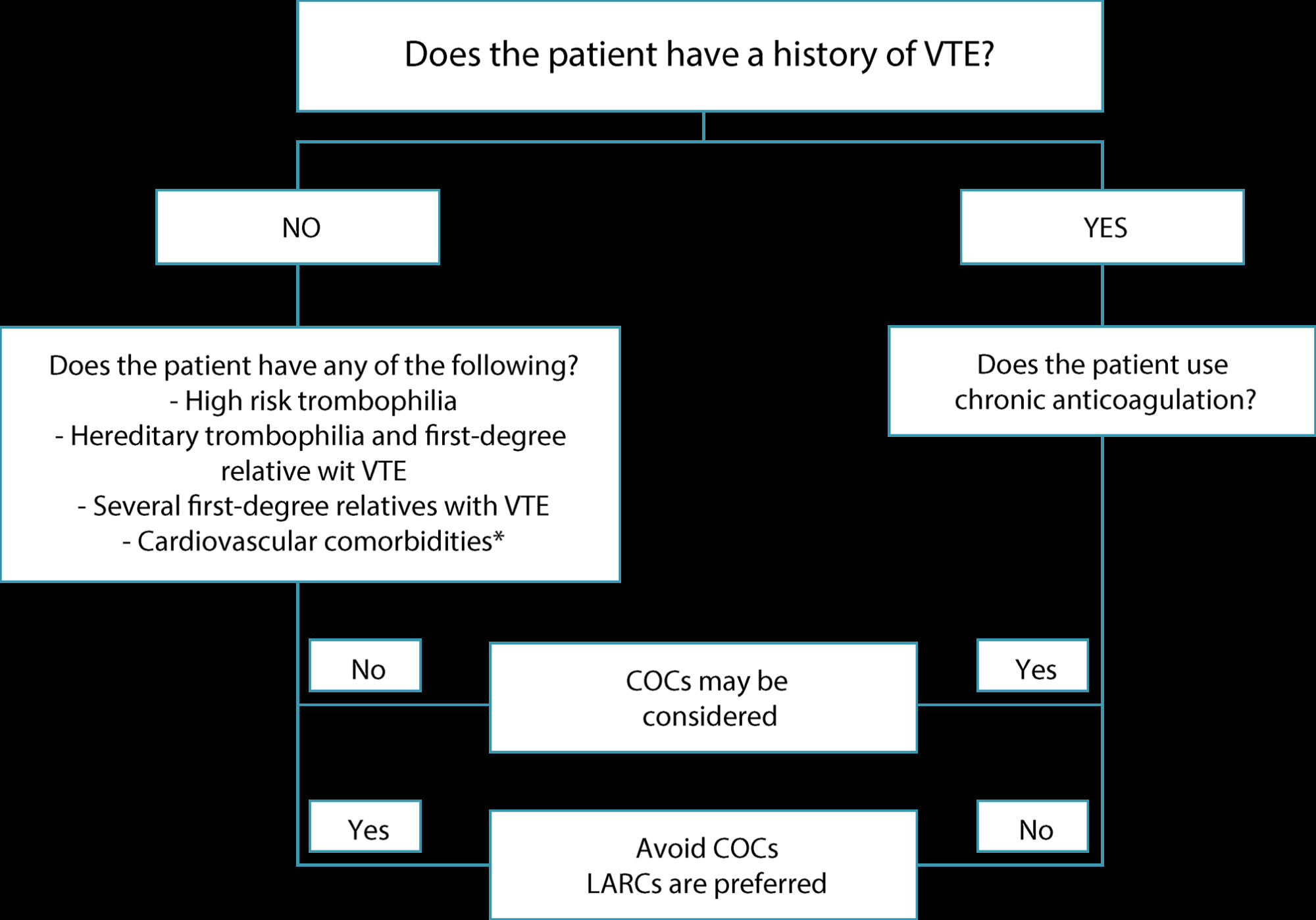
•The risk of venous thromboembolism (VTE) is not increased in women using long-acting reversible contraceptive methods (LARCs) with progestogens.
•Oral contraceptives with levonorgestrel or norgestimate confer half the risk of VTE compared to oral contraceptives containing desogestrel, gestodene or drospirenone.
•Progestogen-only pills do not confer an increased risk of VTE.
•Women using transdermal contraceptive patches and combined oral contraceptives (COCs) are at an approximately eight times greater risk of VTE than non-users of hormonal contraceptives (HCs), corresponding to 9.7 events per 10,000 women/years.
•Vaginal rings increase the risk of VTE by 6.5 times compared to not using HC, corresponding to 7.8 events per 10,000 women/years.
•Several studies have demonstrated an increased risk of VTE in transgender individuals receiving hormone therapy (HT).
•Hormone therapy during menopause increases the risk of VTE by approximately two times, and this risk is increased by obesity, thrombophilia, age over 60 years, surgery and immobilization.
•The route of estrogen administration, the dosage and type of progestogen associated with estrogen may affect the risk of VTE in the climacteric.
•Combined estrogen-progesterone therapy increases the risk of VTE compared to estrogen monotherapy.
•Postmenopausal HT increases the risk of thrombosis at atypical sites.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-FPS03
• The balanced vaginal microbiome is the main factor defending the vaginal environment against infections. Lactobacilli play a key role in this regard, maintaining the vaginal pH within the normal range (3.8 to 4.5).
•Hormonal and immune adaptations resulting from pregnancy influence changes in the vaginal microbiome during pregnancy.
•An altered vaginal microbiome predisposes to human immunodeficiency virus (HIV) infection.
•Bacterial vaginosis is the main clinical expression of an imbalanced vaginal microbiome.
•Vulvovaginal candidiasis depends more on the host’s conditions than on the etiological agent.
•Trichomonas vaginalis is a protozoan transmitted during sexual intercourse.
•The use of probiotics is not approved for use in pregnant women.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-FPS04
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-FPS05
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-FPS06
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo1
To evaluate the association between clinical and imaging with surgical and pathological findings in patients with suspected neuroendocrine tumor of appendix and/or appendix endometriosis.
Retrospective descriptive study conducted at the Teaching and Research Institute of Hospital Israelita Albert Einstein, in which medical records and databases of patients with suspected neuroendocrine tumor of appendix and/or endometriosis of appendix were analyzed by imaging.
Twenty-eight patients were included, all of which had some type of appendix alteration on the ultrasound examination. The pathological outcome of the appendix found 25 (89.3%) lesions compatible with endometriosis and three (10.7%) neuroendocrine tumors. The clinical findings of imaging and surgery were compared with the result of pathological anatomy by means of relative frequency.
It was possible to observe a higher prevalence of appendix endometriosis when the patient presented more intense pain symptoms. The image observed on ultrasound obtained a high positive predictive value for appendicular endometriosis.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo10
To analyze data of patients with symptomatic pelvic organ prolapse evaluated with PFDI20 and its subscales to report the prevalence of lower gastrointestinal symptoms and anal incontinence in the population of a public hospital and analyze its impact on quality of life.
Cross-sectional study of patients with symptomatic POP. Patients were evaluated with demographic data, POP-Q, pelvic floor ultrasonography, urological parameters, and pelvic floor symptoms (PFDI-20), and quality of life (P-QoL) surveys. Patients were classified as CRADI-8 "positive" for colorectal symptoms, with responses "moderate" in at least 3 and/or "severe" in at least 2 of the items in the CRADI-8 questionnaires.
One hundred thirteen patients were included. 42.5% (48) were considered positive for colorectal symptoms on CRADI-8. 53.4% presented anal incontinence. No significant differences were found in sociodemographic variables, POP-Q stage, ultrasound parameters, or urological parameters. Positive patients had a significantly worse result in PFDI-20, POPDI (48 vs 28; p<0.001), UDI6 (51 vs 24; p<0.001), and in the areas of social limitation (44.4 vs 22.2; p = 0.045), sleep- energy (61.5 vs 44.4; p = 0.08), and severity (56.8 vs 43.7, p=0.015) according to P-QoL.
Moderate or severe colorectal symptoms are seen in 40% of patients with symptomatic POP in our unit. Full evaluation of pelvic floor dysfunction symptoms should be performed routinely in urogynecology units.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2024;46:e-rbgo11
To show the experience of a Latin American public hospital, with SNM in the management of either OAB, NOUR or FI, reporting feasibility, short to medium-term success rates, and complications.
A retrospective cohort was conducted using data collected prospectively from patients with urogynecological conditions and referred from colorectal surgery and urology services between 2015 and 2022.
Advanced or basic trial phases were performed on 35 patients, 33 (94%) of which were successful and opted to move on Implantable Pulse Generator (GG) implantation. The average follow-up time after definitive implantation was 82 months (SD 59). Of the 33 patients undergoing, 27 (81%)reported an improvement of 50% or more in their symptoms at last follow-up. Moreover, 30 patients (90%) with a definitive implant reported subjective improvement, with an average PGI-I "much better" and 9 of them reporting to be "excellent" on PGI-I.
SNM is a feasible and effective treatment for pelvic floor dysfunction. Its implementation requires highly trained groups and innovative leadership. At a nation-wide level, greater diffusion of this therapy among professionals is needed to achieve timely referral of patients who require it.