You searched for:"Renato Luis Rombaldi"
We found (8) results for your search.Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(7):330-336
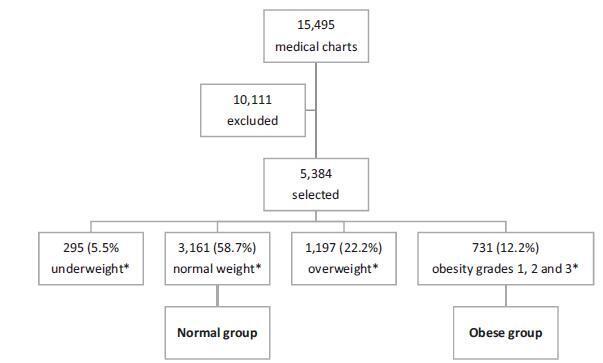
To assess the impact of pre-pregnancy obesity (body mass index [BMI] ≥30 kg/m2) on the gestational and perinatal outcomes.
Retrospective cohort study of 731 pregnant women with a BMI ≥30 kg/m2 at the first prenatal care visit, comparing them with 3,161 women with a BMI between 18.5 kg/m2 and 24.9 kg/m2. Maternal and neonatal variables were assessed. Statistical analyses reporting the demographic features of the pregnant women (obese and normal) were performed with descriptive statistics followed by two-sided independent Student’s t tests for the continuous variables, and the chi-squared (χ2) test, or Fisher’s exact test, for the categorical variables. We performed a multiple linear regression analysis of newborn body weight based on the mother’s BMI, adjusted by maternal age, hyperglycemic disorders, hypertensive disorders, and cesarean deliveries to analyze the relationships among these variables. All analyses were performed with the R (R Foundation for Statistical Computing, Vienna, Austria) for Windows software, version 3.1.0. A value of p < 0.05 was considered statistically significant.
Obesity was associated with older age [OR 9.8 (7.8-12.2); p < 0.01], hyperglycemic disorders [OR 6.5 (4.8-8.9); p < 0.01], hypertensive disorders [OR 7.6 (6.1-9.5); p < 0.01], caesarean deliveries [OR 2.5 (2.1-3.0); p < 0.01], fetal macrosomia [OR 2.9 (2.3-3.6); p < 0.01] and umbilical cord pH [OR 2.1 (1.4-2.9); p < 0.01). Conversely, no association was observed with the duration of labor, bleeding during labor, Apgar scores at 1 and 5 minutes after birth, gestational age, stillbirth and early neonatal mortality, congenital malformations, and maternal and fetal injury.
We observed that pre-pregnancy obesity was associated with maternal age, hyperglycemic disorders, hypertension syndrome, cesarean deliveries, fetal macrosomia, and fetal acidosis.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(11):516-522
DOI 10.1590/S0100-72032013001100007
PURPOSE: To analyze the impact of vaginal delivery after a previous cesarean section on perinatal outcomes. METHODS: Case-control study with selection of incident cases and consecutive controls. Maternal and perinatal variables were analyzed. We compared secundiparas who had a vaginal delivery after a previous cesarean delivery (VBAC) (n=375) with secundiparas who had a second cesarean section (CS) (n=375). Inclusion criteria were: secundiparas who underwent a cesarean section in the previous pregnancy; singleton and term pregnancy; fetus in vertex presentation, with no congenital malformation; absence of placenta previa or any kind of bleeding in the third quarter of pregnancy. RESULTS: The rate of vaginal delivery was 45.6%, and 20 (5.3%) women had forceps deliveries. We found a significant association between VBAC and mothers younger than 19 years (p<0.01), Caucasian ethnicity (p<0.05), mean number of prenatal care visits (p<0.001), time of premature rupture of membranes (p<0.01), labor duration shorter than 12 hours (p<0.04), Apgar score lower than seven at 5th minute (p<0.05), fetal birth trauma (p<0.01), and anoxia (p<0.006). In the group of newborns delivered by cesarean section, we found a higher frequency of transient tachypnea (p<0.014), respiratory disorders (p<0.048), and longer time of stay in the neonatal intensive care unit (p<0.016). There was only one case of uterine rupture in the VBAC group. The rate of neonatal mortality was similar in both groups. CONCLUSIONS: Vaginal delivery in secundiparas who had previous cesarean sections was associated with a significant increase in neonatal morbidity. Further studies are needed to develop strategies aimed at improving perinatal results and professional guidelines, so that health care professionals will be able to provide their patients with better counseling regarding the choice of the most appropriate route of delivery.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(8):381-385
DOI 10.1590/S0100-72032012000800007
PURPOSE: To assess perinatal factors associated with term newborns with pH<7.1 in the umbilical artery and 5th min Apgar score<7,0. METHODS: Retrospective case-control study carried out after reviewing the medical records of all births from September/1998 to March/2008, that occurred at the General Hospital of Caxias do Sul. The inclusion criterion was term newborns who presented a 5th min Apgar score <7.0 and umbilical artery pH<7.10. In the univariate analysis, we used the Student's t-test and the Mann-Whitney test for continuous variables, the c² test for dichotomous variables and risk estimation by the odds ratio (OR). The level of significance was set at p<0.05. RESULTS: Of a total of 15,495 consecutive births, 25 term neonates (0.16%) had pH<7.1 in the umbilical artery and a 5th min Apgar score <7.0. Breech presentation (OR=12.9, p<0.005), cesarean section (OR=3.5, p<0.01) and modified intrapartum cardiotocography (OR=7.8, p<0.02) presented a significant association with the acidosis event. Among the fetal characteristics, need for hospitalization in the neonatal intensive care unit (OR=79.7, p <0.0001), need for resuscitation (OR=12.2, p <0.0001) and base deficit were associated with the event (15.0 versus -4.5, p<0.0001). CONCLUSION: Low Apgar score at the 5th min of life associated with pH<7.1 in the umbilical artery can predict adverse neonatal outcomes.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2009;31(1):10-16
DOI 10.1590/S0100-72032009000100003
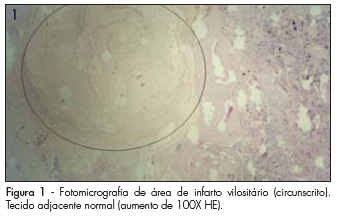
PURPOSE: to determine the prevalence of histopathological changes, in human placentas, related to hypertensive syndromes. METHODS: a transversal study that compares histopathological changes identified in 43 placentae from hypertensive pregnant women (HypPr), with the ones from 33 placentae from normotensive pregnant women (NorPr). The weight, volume and macroscopic and microscopic occurrence of infarctions, clots, hematomas, atherosis (partial obliteration, thickness of layers and presence of blood vessels hyalinization) and Tenney-Parker changes (absent, discreet and prominent), as well as the locating of infarctions and clots (central, peripheral or the association of both) have been analyzed. The χ2 and t Student tests have been used for the statistical analysis, as well as medians, standard deviations and ratios. It has been considered as significant, p<0.05. RESULTS: the macroscopic study of HypPr placentae have presented lower weight (461.1 versus 572.1 g) and volume (437.4 versus 542.0 cm³), higher infarction (51.2 versus 45.5%; p<0.05: OR=1.15) and clots (51.2 versus 15.1%; p<0.05; OR=5.4) ratios, as compared to the NorPr's. In the HypPr and NorPr, microscopic clots have occurred in 83.7 versus 45.5% (p<0.05; OR=4.3), respectively. Atherosis and Tenney-Parker changes have been statistically associated to the hypertensive syndromes (p<0.05). CONCLUSIONS: the obtained data allow us to associate lower placentary weight and volume, higher ratio of macro and microscopic infarction, clots, atherosis and Tenney-Parker changes to placentae of gestations occurring with hypertensive syndromes.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(4):232-237
DOI 10.1590/S0100-72032006000400005
PURPOSE: to identify maternal and perinatal factors related to neonates with birthweight >4,000 g. METHODS: cross-section cohort study with 411 consecutive cases of fetal macrosomia (FM) which occurred from March 1998 to March 2005. Data were compared to 7,349 cases of fetal birthweight >2,500 and <3,999 g which occurred in the same period. Maternal variables (maternal age, parity, diabetes, previous cesarean section, meconium-stained amniotic fluid, cephalopelvic disproportion, main cesarean section indications) and perinatal variables (birth injury, <7 1-min and 5-min Apgar score, fetal and early neonatal mortality range, need of neonatal intensive care unit) were analyzed. For statistical analysis the chi2 test with Yates correction and Student's t test were used with the level of significance set at 5%. RESULTS: FM was significantly associated with older mothers, more parous and <7 1-min Apgar score (p<0.05; OR=1.8; 95% CI: 1,4-2.5) and <7 5-min Apgar score (p<0,05; OR=2.3; 95% CI: 1.3-4,1), diabetes mellitus (p<0.05; OR=4.2; 95% CI: 2.7-6.4), meconium-stained amniotic fluid (p<0.02; OR=1.3; 95% CI: 1.0-1.7), need of neonatal intensive care unit (p<0,05; OR=2.0; 95% CI: 1.5-2.7), early neonatal mortality (p<0,05; OR = 2.7; 95% CI: 1.0-6.7), cesarean section (p < 0.05; OR = 2.03; 95% CI: 1,6-2,5) and cephalopelvic disproportion (p < 0.05;OR = 2.8; 95% CI: 1.6-4,8). There was no statistical difference between birth injury and fetal mortality range. In the FM group the main cesarean section indications were repeat cesarean sections (11.9%) and cephalopelvic disproportion (8.6%); in the normal birthweight group, repeat cesareans (8.3%) and fetal distress during labor (3.9%). CONCLUSIONS: in spite of the characteristic limitations of a retrospective evaluation, the analysis demonstrated which complications were associated with large fetal size, being useful in obstetric handling of patients with a diagnosis of extreme fetal growth. FM remains an obstetric problem of difficult solution, associated with important maternal and perinatal health problems, due to the significant observed rates of maternal and perinatal morbidity and mortality in developed and developing countries.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(2):75-79
DOI 10.1590/S0100-72032005000200006
PURPOSE: to evaluate perinatal outcomes in cases of oligohydramnios without premature rupture of membranes. METHODS: a total of 51 consecutive cases of oligohydramnios (amniotic fluid index, AFI < 5 cm) born between March 1998 and September 2001 were studied retrospectively. Data were compared to 61 cases with intermediate and normal volume of amniotic fluid AFI >5). Maternal and neonatal variables, as well as fetal mortality, early neonatal, and perinatal mortality rates were analyzed. For statistical analysis the c² test with Yates correction and Student's t test were used with level of signicance set at 5%. RESULTS: there were no significant differences between groups when the presence of gestational hypertensive syndromes, meconium-stained amniotic fluid, 1- and 5-minute Apgar score, need of neonatal intensive center unit, and preterm birth were analyzed. Oligohydramnios was associated with the way of delivery (p<0.0002; RR=0.3), fetal distress (p<0.0004; RR=2.2) and fetal malformations (p<0.01; RR=5.4). Fetal malformation rates were 17.6 and 3.3% in oligohydramnios and normal groups, respectively. Fetal mortality (2.0 vs 1.6%), early neonatal (5.9 vs 1.6%) and perinatal mortality (7.8 vs 3.3%) rates in both groups did not show statistical significance. CONCLUSION: Oligohydramnios was related to increased risk factor for cesarean section, fetal distress and fetal malformations.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2004;26(10):781-786
DOI 10.1590/S0100-72032004001000005
PURPOSE: to assess the obstetric and perinatal outcomes in cases of term newborns in breech presentation, in patients with previous vaginal deliveries, comparing them to term newborns in vertex presentation. METHODS: 8,350 deliveries retrospectively from March 1998 to July 2003 were analysed. Of 419 deliveries (5.1%) in breech presentation, 58 cases were selected for the study (breech group), according to the following criteria: patients who had had one or more babies through vaginal delivery, gestational age ³37 weeks, no fetal malformation, no complications in the current pregnancy, birth weight between 2,500 and 3,750 g, and no previous cesarean section. The breech group was matched to 1,327 newborns in vertex position from pregnant women with no previous cesarean section (vertex group). Maternal age, parity, gestational age, delivery way, birth weight, meconium-stained amniotic fluid, 1- and 5-min Apgar score, need of neonatal intensive care unit, and small- and big-for-gestational age newborns were analyzed. Statistical analysis was performed by the c² test and by Student's t test, with the level of significance set at p<0.05. RESULTS: when breech and vertex groups were compared, they showed significant differences regarding the following variables: birth weight (3,091±538 g vs 3,250±497 g; p<0.01), vaginal delivery (63.8 vs 95.0%; p<0.0001), cesarean section (36.2 vs 5.0%; p<0,0001), and 1-min Apgar score (p<0.0001), respectively. CONCLUSIONS: we conclude that in term fetuses in breech position from pregnant women with previous vaginal deliveries, birth weight, delivery way, and 1-min Apgar score were different compared to fetuses in vertex position from women with the same characteristics.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(2):123-128
DOI 10.1590/S0100-72032003000200008
PURPOSE: to analyze obstetrical and perinatal data in 26 cases of meconium aspiration syndrome (MAS). METHODS: a retrospective review was performed in 26 newborn records diagnosed with meconium aspiration syndrome. Patients were studied emphasizing average days in neonatal intensive care unit and main maternal findings and neonatal complications, correlating them with each other. RESULTS: Eighteen babies were delivered at GH-CSUF and eight out of this hospital. At this time 3,976 deliveries occurred at GH-CSUF, with an incidence of MAS of 0.45%. Nine of 18 babies were born by vaginal delivery; weight was >2,500 g in 16 cases. One-minute Apgar score was >7 in three cases (16.7%), between 4 and 6 in seven cases (38.9%), and between 0 and 3, in eight cases (44.4%). At 5 minutes, seven babies remained <7. Anoxia was the main neonatal complication (36%). The mortality rate was 7.7% and the average hospital stay was 19.9 days. CONCLUSION: MAS is a very important neonatal pathology correlated with high neonatal mortality rates, thick meconium in at least half of the cases, and with a majority of depressed newborns at delivery.