Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(5):240-247
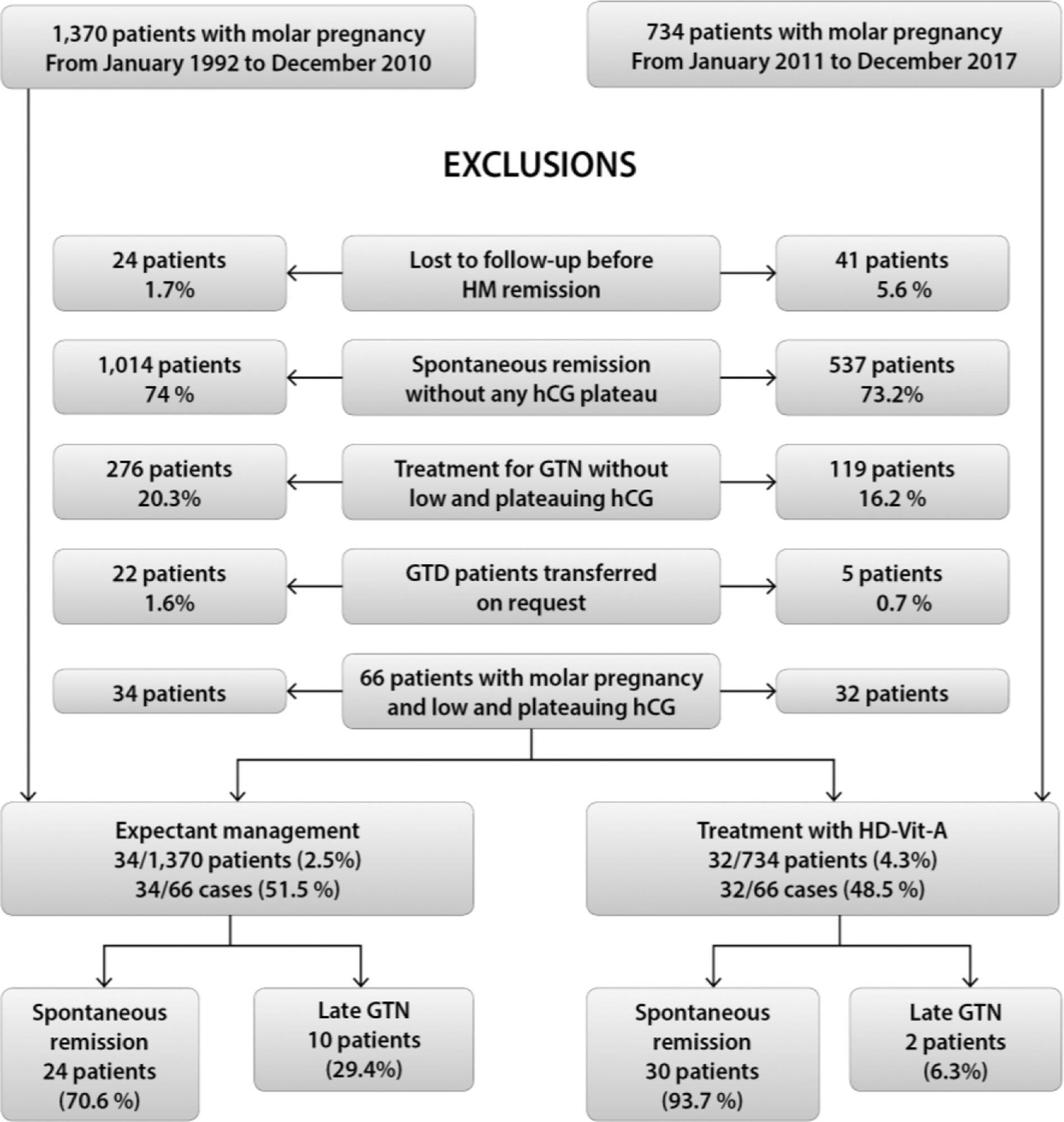
To compare the effect of high-dose vitamin A (HD Vit-A) use during postmolar follow-up of patients with low and plateauing (L&P) serum human chorionic gonadotropin (hCG) levels, from the moment serum hCG plateaued (P-hCG) to the first normal serum hCG value (< 5IU/L).
The present retrospective series case study compared two nonconcurrent cohorts of patients. Control group (CG): 34 patients with L&P serum hCG levels who underwent expectant management for 6 months after uterine evacuation, from 1992 to 2010; study group (SG): 32 patients in similar conditions who received 200,000 IU of Vit-A daily, from the identification of a P-hCG level to the first normal hCG value or the diagnosis of progression to gestational trophoblastic neoplasia (GTN), from 2011 to 2017. The present study was approved by the Ethics Committee of the institution where it was conducted.
In both groups, the prevalence of persistent L&P serum hCG levels was < 5%. In the SG, hCG levels at plateau were higher (CG = 85.5 versus SG = 195 IU/L; p = 0.028), the rate of postmolar GTN was lower (CG = 29.4% versus SG = 6.3%, p = 0.034) and follow-up was shorter (CG = 14 versus SG = 10 months, p < 0.001). During GTN follow-up, there were no differences in GTN staging or treatment aggressiveness in both groups. High-dose Vit-A use did not have any relevant toxic effect. There were no GTN relapses or deaths.
The limited use of HD Vit-A seems to have a safe and significant effect on the treatment of postmolar patients with L&P serum hCG levels and may decrease the development of postmolar GTN in this population.

Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(5):235-239
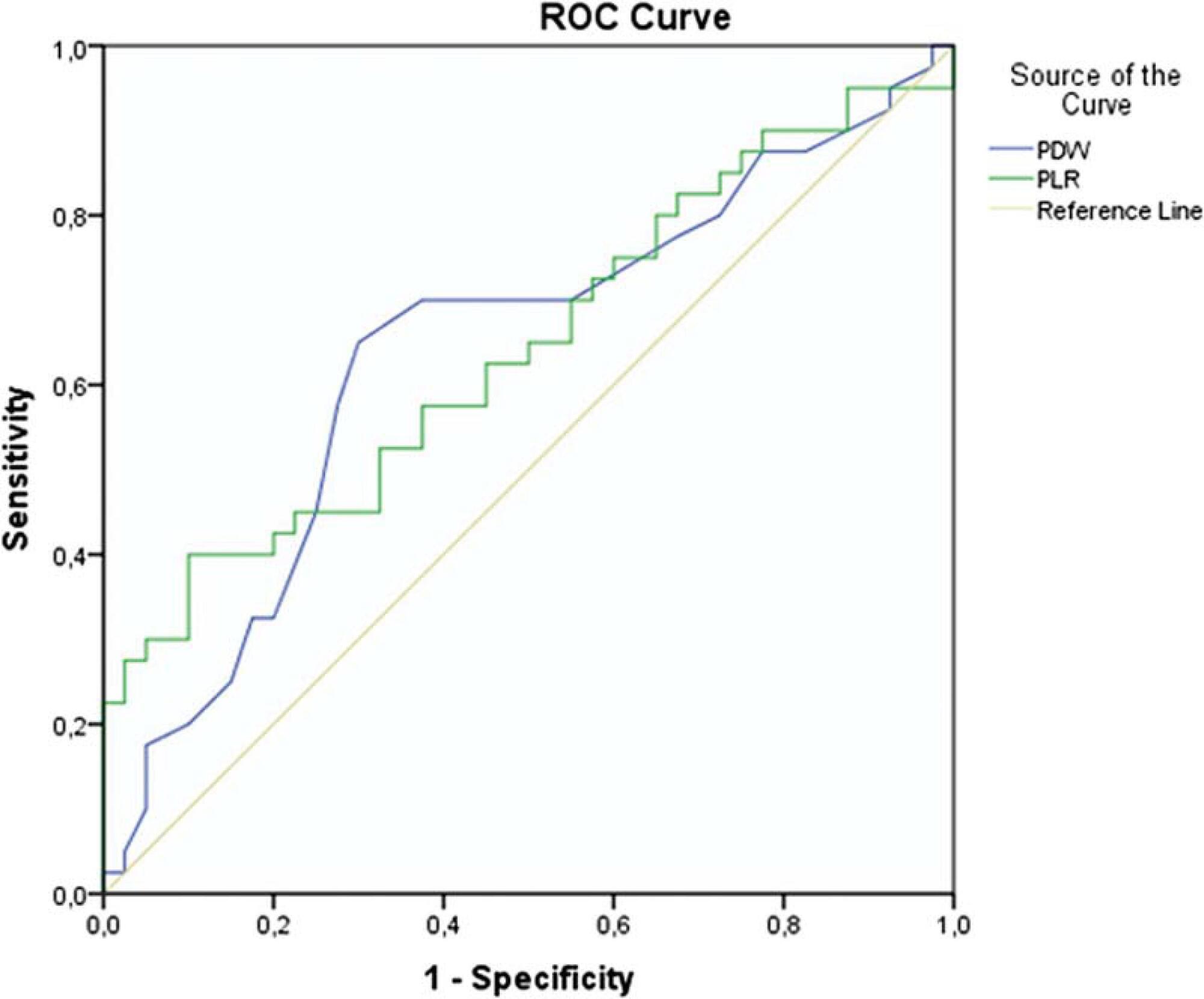
Missed abortion occurs in ~ 15% of all clinical pregnancies. The pathogenesis is not clearly known. However, defective placentation resulting in maternal systemic inflammatory response is considered responsible for missed abortion. Platelet lymphocyte ratio (PLR) and neutrophil lymphocyte ratio (NLR) are increasingly cited parameters of inflammation in the literature. However, no study evaluated the PLR and NLR rates in missed abortions so far. The aim of the present study is to investigate whether complete blood count (CBC) inflammatory parameters such as NLR and PLR are increased in patients with missed abortion.
Medical records of 40 pregnant women whose gestation ended in missed abortion at between 6 and14 weeks of gestation and of 40 healthy pregnant women were collected and compared retrospectively. The groups were compared regarding hemoglobin, hematocrit, platelet count (PLT), mean platelet volume (MPV), platelet distribution width (PDW), PLR and NLR.
Platelet distribution width, NLR and PLR values were higher in the missed abortion group compared with the healthy pregnant women group (rates are p = 0.043; p = 0.038; and p = 0.010, respectively). Hematocrit, MPV, and lymphocyte values were found to be lower in the missed abortion group compared with the healthy pregnant women group (p = 0.027, p = 0.044 and p = 0.025, respectively).
The PDW, NLR and PLR values of the missed abortion group were reported high; and MPV values were reported low in the present study. These findings may help to speculate a defective placentation in the pathogenesis of missed abortion.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(4):211-217
To reveal the changes in the quality of life reported by women with Human papillomavirus (HPV)-induced lesions.
This is a cross-sectional, descriptive-exploratory study of a qualitative approach performed from June to August 2016. Semi-structured face-to-face interviews based on five questions on the concept of quality of life were used. The data were submitted to thematic analysis. All ethical aspects have been contemplated.
A total of 20 women aged between 25 and 59 years old were interviewed. From the analysis of the data, the following thematic units emerged: physical and emotional changes, especially complaints of pruritus, discharge and pain, worry, fear, shame and sadness; changes in sexual and affective relationships with decreased libido, dyspareunia and interruption of sexual activity; changes in social relationships resulting in absenteeism at work.
Human papillomavirus infection impairs the quality of life of women as it significantly affects sexual, affective, physical, emotional, and everyday habits. Therefore, HPV infection can lead to exponential changes in the quality of life of women, which can be mitigated by the availability of sources of support such as family, friends and the multi-professional team, helping to improve knowledge and cope with HPV.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(4):200-210
The present study is a systematic review of the literature to assess whether the presence of endometriosis determines or contributes to adverse obstetric outcomes.
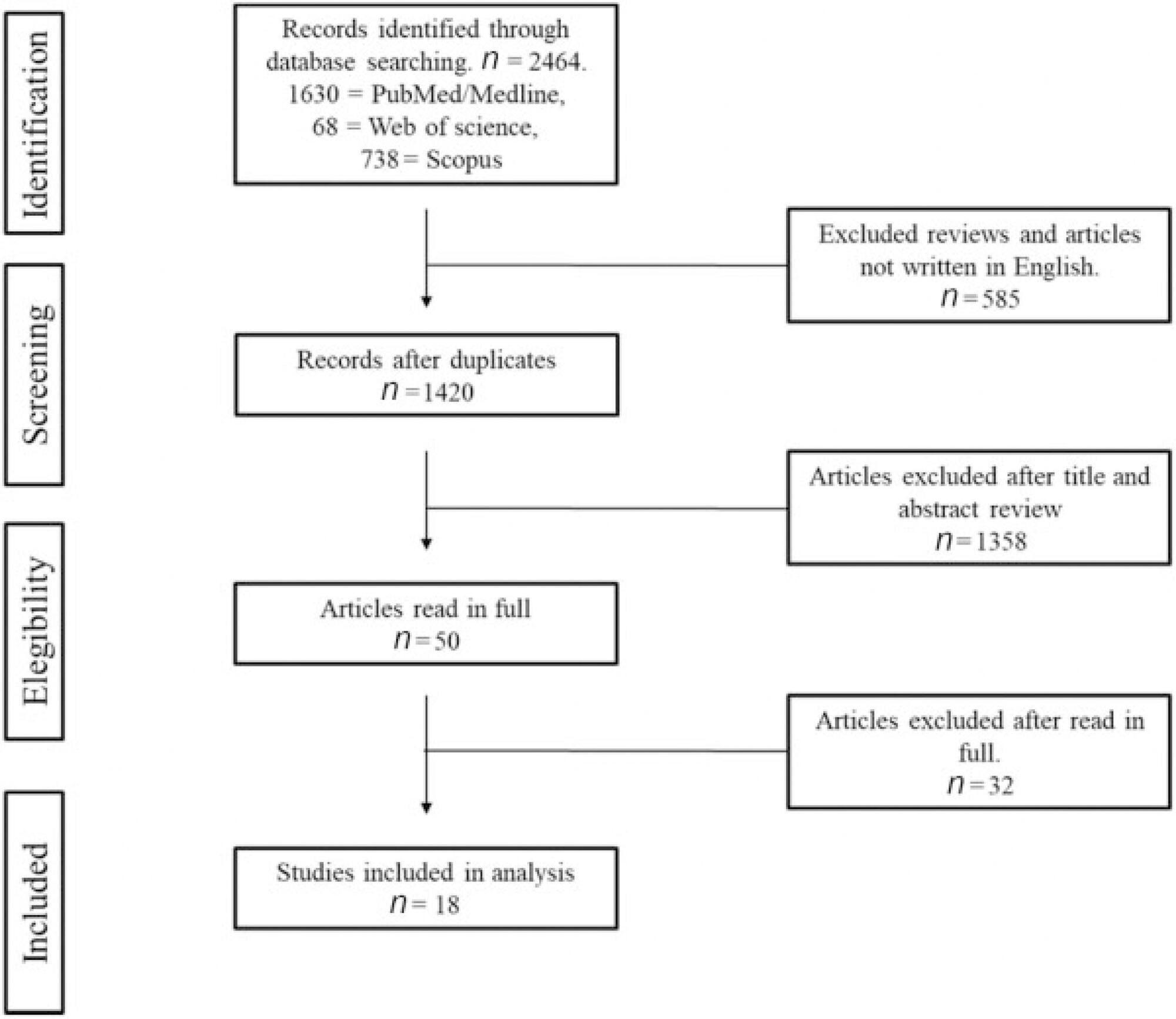
The present work was carried out at the Hospital Israelita Albert Einstein, São Paulo, state of São Paulo, Brazil, in accordance to the PRISMA methodology for systematic reviews. A review of the literature was performed using PubMed, Web of Science and Scopus databases. The keywords used were: pregnancy outcome, pregnancy complications, obstetrical complications, obstetrics, obstetric outcomes and endometriosis. The survey was further completed by a manually executed review of cross-referenced articles, which was last performed on November 30, 2018.
The survey disclosed a total of 2,468 articles, published from May 1946 to October 2017. A total of 18 studies were selected to be further classified according to their quality and relevance.
The Newcastle-Ottawa Quality Assessment Scale was used for classification. Five studies of greater impact and superior evidence quality and 13 studies of moderate evidence quality were selected. We analyzed the studies for the characteristics of their patients plus how endometriosis was diagnosed and their respective obstetric outcomes taking into account their statistical relevance.
Analyses of the higher impact and better quality studies have shown high incidence of preterm birth and placenta previa in patients with endometriosis.
Placenta previa and preterm birth are the most statistically significant outcomes related to endometriosis, as indicated by our systematic review. The present information is useful to alert obstetricians and patients about possible unfavorable obstetric outcomes.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(4):194-199
Changes in bleeding patterns could influence the decisions of healthcare professionals to change the levonorgestrel-releasing intrauterine system (LNG-IUS) before 7 years of use, the recommended period of extended use. We evaluated changes in the bleeding patterns of users of the 52 mg LNG-IUS at the end of use of the first (IUS-1) and during the second device (IUS-2) use.
We performed an audit of the medical records of all women who used two consecutive LNG-IUSs at the Family Planning clinic. We evaluated the sociodemographic/gynecological variables, the length of use, and the bleeding patterns reported in the reference periods of 90 days before removal of the IUS-1 and at the last return in use of IUS-2. We used the McNemar test to compare bleeding patterns. Statistical significance was established at p < 0.05.
We evaluated 301 women aged (mean ± SD) 32 (±6.1) years, with lengths of use of 68.9 (±16.8) and 20.3 (±16.7) months for the IUS-1 and IUS-2, respectively. No pregnancies were reported. Bleeding patterns varied significantly among women who used the IUS-2 for ≥ 7 months to 6 years when compared the bleeding patterns reported in IUS-1 use. Eighty-nine out of 221 (40%) women maintained amenorrhea and infrequent bleeding; 66 (30%) evolved to bleeding patterns with light flow, and 66 (30%) maintained or evolved to heavy flow patterns (p = 0.012). No differences were observed among the 80 women with ≤ 6 months of use.
Changes in bleeding patterns occur during the use of LNG-IUS and should not be decisive for the early replacement of the device.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(4):188-193
To evaluate the frequency of structural congenital anomalies (CAs) in the midwest of Brazil and its association with maternal risk factors.
This was a prospective, observational, case-control study based on a hospital population. Pregnant women attended at a fetal medicine service in Brazil were analyzed in the period from October 2014 to February 2016.A total of 357 pregnant women were included, 223 of whom had fetuses with structural anomalies (group case), and 134 of whom had structurally normal fetuses (control group). The clinical history was made previous to prenatal consultation, and the diagnosis of the structural CA was performed through ultrasound.
A frequency of 64.27% (n = 223) of pregnant women with fetuses with structural anomalies was observed. The most frequent structural CAs were those of the central nervous system (30.94%), followed by anomalies of the genitourinary system (23.80%), and, finally, by multiple CAs (16.60%). The background of previous children with CAs (odds ratio [OR]: 3.85; p = 0.022), family history (OR: 6.03; p = < 0.001), and consanguinity between the progenitors (OR: 4.43; p = 0.034) influenced the occurrence of structural CA.
The most frequent CAs are those of the central nervous system, followed by those of the genitourinary system, and then multiple anomalies. The maternal risk factors that may have influenced the occurrence of structural CA were previous children with CA, family history, and consanguinity among the parents.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(4):181-187
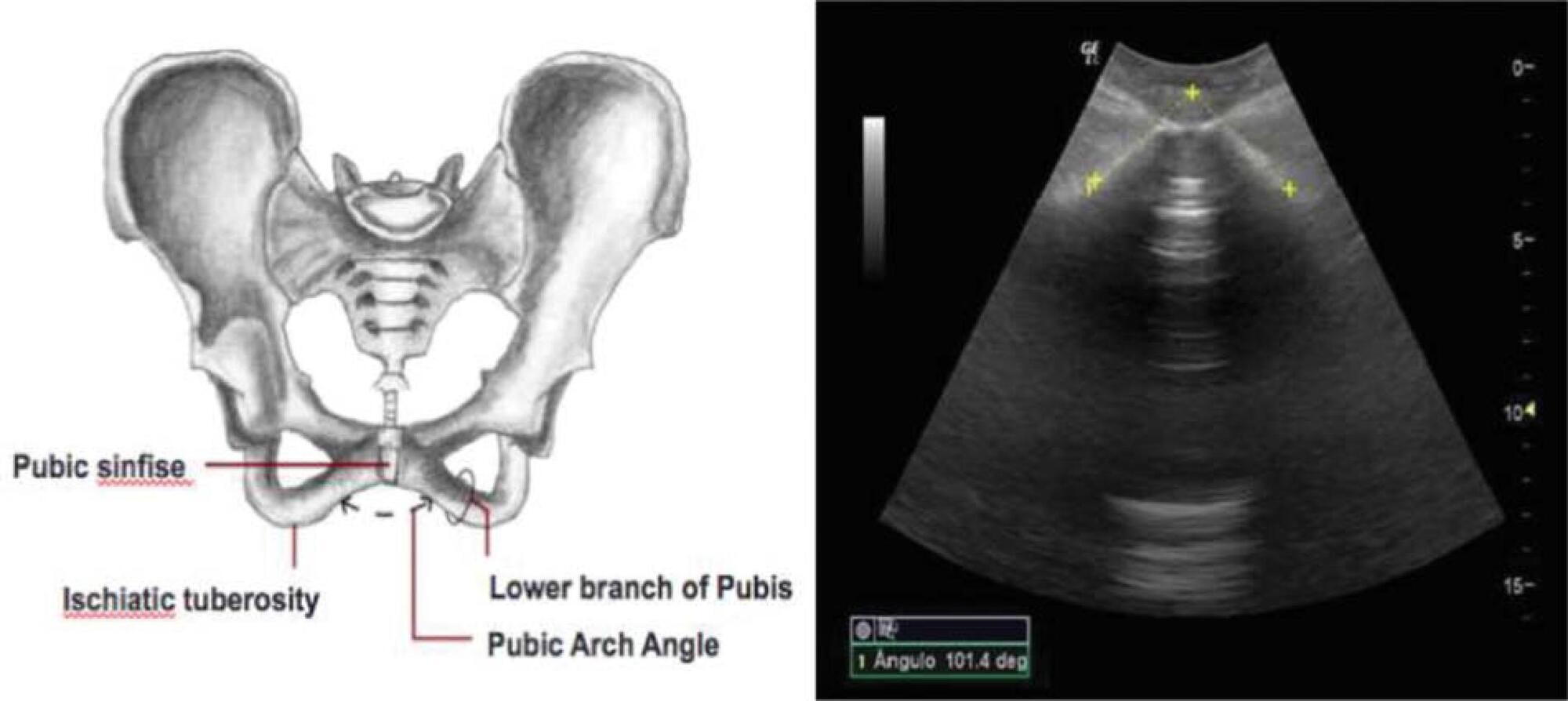
To evaluate the ability of the pubic arch angle (PAA) as measured by transperineal ultrasonography during labor to predict the delivery type and cephalic pole disengagement mode.
The present prospective cross-sectional study included 221 women in singleton-gestational labor ≥ 37 weeks with cephalic fetuses who underwent PAA measurement using transperineal ultrasonography. These measurements were correlated with the delivery type, cephalic pole disengagement mode, and fetal and maternal characteristics.
Out of the subjects, 153 (69.2%) had spontaneous vaginal delivery, 7 (3.2%) gave birth by forceps, and 61 (27.6%) delivered by cesarean section. For the analysis, deliveries were divided into two groups: vaginal and surgical (forceps and cesarean). The mean PAA was 102 ± 7.5º (range, 79.3-117.7º). No statistically significant difference was observed in delivery type (102.6 ± 7.2º versus 100.8 ± 7.9º, p = 0.105). The occipitoanterior position was seen in 94.1% of the fetuses and the occipitoposterior position in 5.8%. A narrower PAA was found in the group of surgical deliveries (97.9 ± 9.6º versus 102.6 ± 7.3º, p = 0.049). Multivariate regression analysis showed that PAA was a predictive variable for the occurrence of head disengagement in occipital varieties after birth (odds ratio, 0.9; 95% confidence interval, 0.82-0.99; p = 0.026).
Ultrasonographic measurement of the PAA was not a predictor of delivery type, but was associated with the persistence of occipital varieties after birth.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(4):174-180
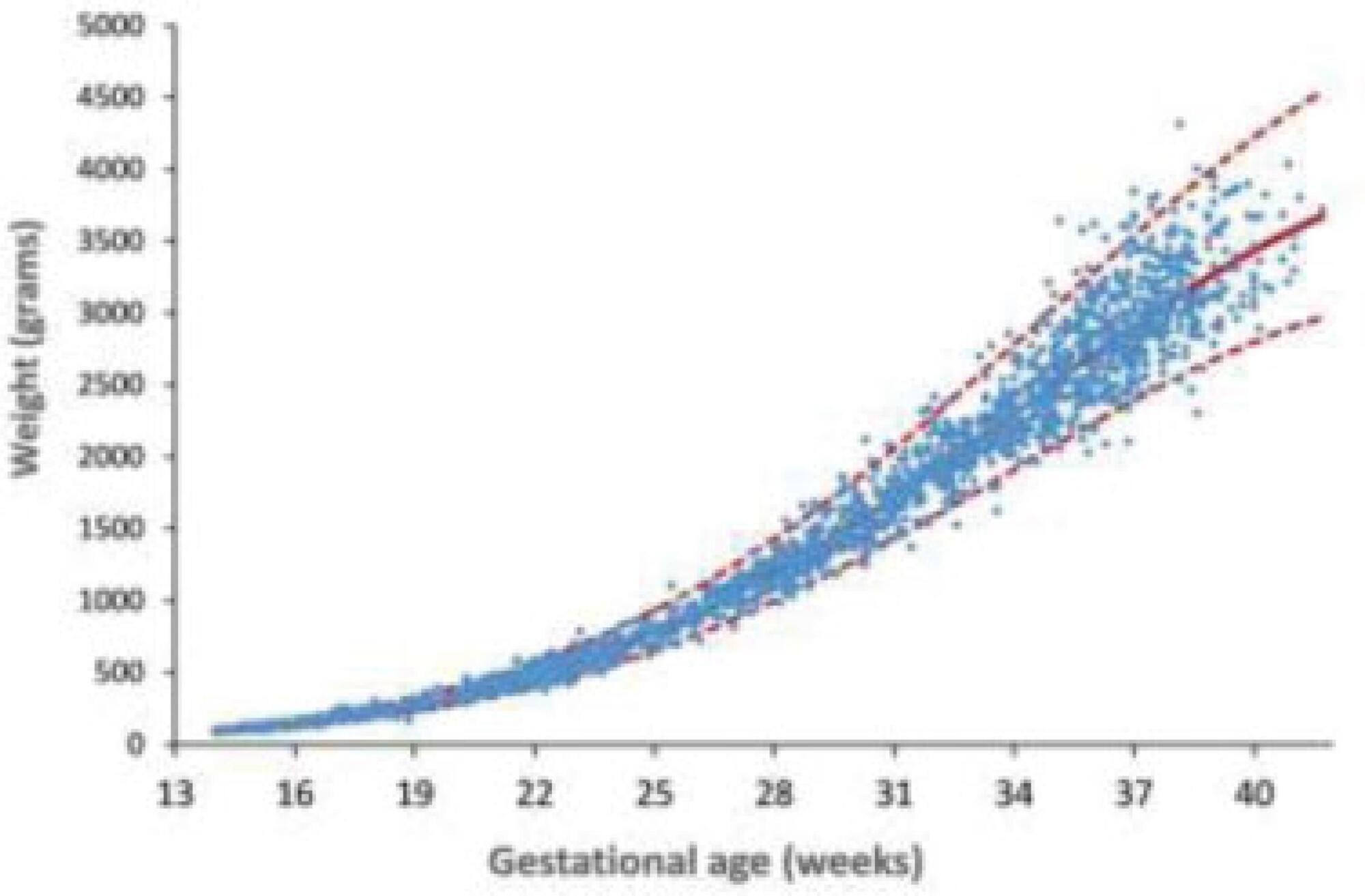
To develop reference curves of estimated fetal weight for a local population in Curitiba, South of Brazil, and compare them with the curves established for other populations.
An observational, cross-sectional, retrospective study was conducted. A reference model for estimated fetal weight was developed using a local sample of 2,211 singleton pregnancies with low risk of growth disorders and well-defined gestational age. This model was compared graphically with the Hadlock and Intergrowth 21st curves.
Reference curves for estimated fetal weight were developed for a local population. The coefficient of determination was R2 = 99.11%, indicating that 99.11% of the fetal weight variations were explained by the model. Compared with Hadlock curves, the 50th, 90th, and 97th percentiles in this model were lower, whereas the 10th percentile nearly overlapped, and the 3rd percentile was slightly higher in the proposed model. The percentiles were higher in the proposed model compared with the Intergrowth 21st curves, particularly for the 3rd, 10th, and 50th percentiles.
We provide a local reference curve for estimated fetal weight. The proposed model was different from other models, and these differences might be due to the use of different populations for model construction.