Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(11):646-653
Currently, uteroplacental vascular disorders are considered one of the main mechanisms of spontaneous preterm delivery (PTD). Low-dose aspirin is used to prevent pre-eclampsia, which has a similar mechanism; hence, the present study aimed to investigate the effect of low-dose aspirin on the prevention of PTD in women with a history of spontaneous PTD.
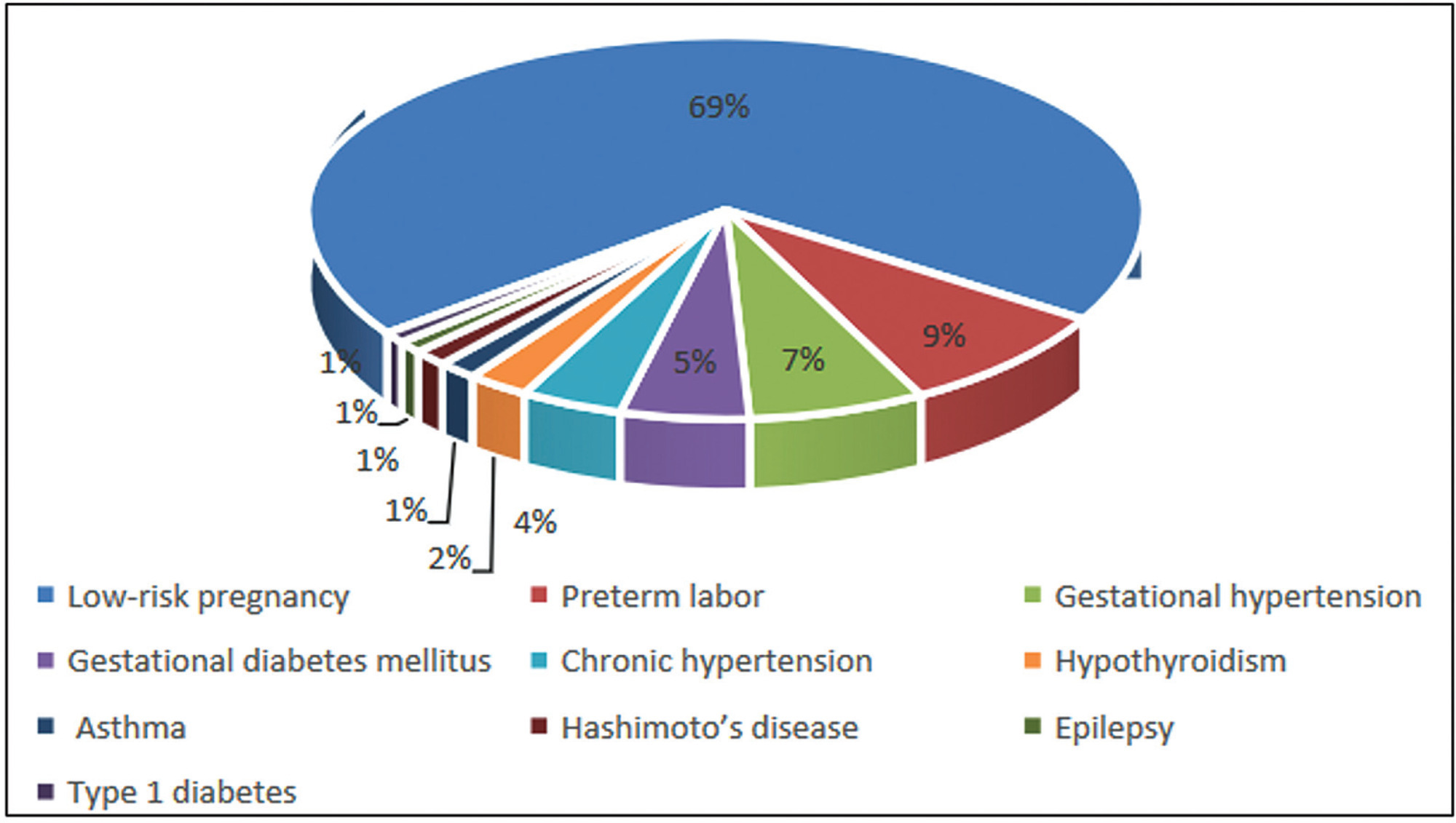
The present pilot randomized clinical trial was conducted on 54 pregnant women in the aspirin group (taking 80 mg daily until the 36th week and classic treatment) and 53 patients in the control group (only receiving classic treatment).
Forty-three patients (40%) presented before 37 weeks due to symptoms of PTL. Preterm delivery (< 37 weeks) occurred in 28 patients (26%), and there was no significant difference between the aspirin and control groups (10 patients [19%] and 18 patients [34%], respectively; p = 0.069). The time of preterm delivery was early (< 34 weeks) in 6 patients (21%), and its cause was spontaneous labor in 23 patients (82%) which was not significantly different between the two groups (p > 0.05). Out of 40 patients with spontaneous labor, 25 patients (63%) had a PTD, which was significantly lower in the aspirin group than in the control group (9 patients [45%] versus 16 patients [80%], respectively; p = 0.022).
The findings of the present study demonstrated that despite the reduction in the incidence of PTD using low-dose aspirin, the reduction rate was not statistically significant. On the other hand, in patients with spontaneous labor prone to PTD, aspirin was effective in reducing the incidence of PTD.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(11):638-645
This study focused on pregnant and postpartum women during the COVID-19 pandemic, aiming to determine the attitudes and behaviors of vaccinated and unvaccinated groups, and the vaccination behaviors in the groups with and without the disease. The reasons for refusing the vaccine were also questioned.
This cross-sectional study was performed from September 2021 to October 2021. The study data were collected using a face-to-face questionnaire. The participants were pregnant women who applied to the hospital for routine antenatal care and were hospitalized, and women in the postpartum period. Additionally, pregnant and postpartum patients who were diagnosed with COVID-19 at the time of admission and were hospitalized and admitted to the intensive care unit due to this disease were also included in the study.
A total of 1,146 pregnant and postpartum women who completed the questionnaire were included in our study. Only 43 (3.8%) of the participants were vaccinated; 154 (13.4%) of the participants had comorbidities. The number of COVID-19-positive patients was 153. The lack of sufficient information about the safety of the COVID-19 vaccine is the most common reason for the refusal.
Vaccine refusal can significantly delay or hinder herd immunity, resulting in higher morbidity and mortality. Considering the adverse effects of COVID-19 on pregnancy, it is essential to understand pregnant and postpartum women's perceptions toward vaccination to end the pandemic.