Home
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2014;36(11):489-496
DOI 10.1590/S0100-720320140005090
To evaluate the predictive clinical factors for the development of endometrial polyps in postmenopausal women.
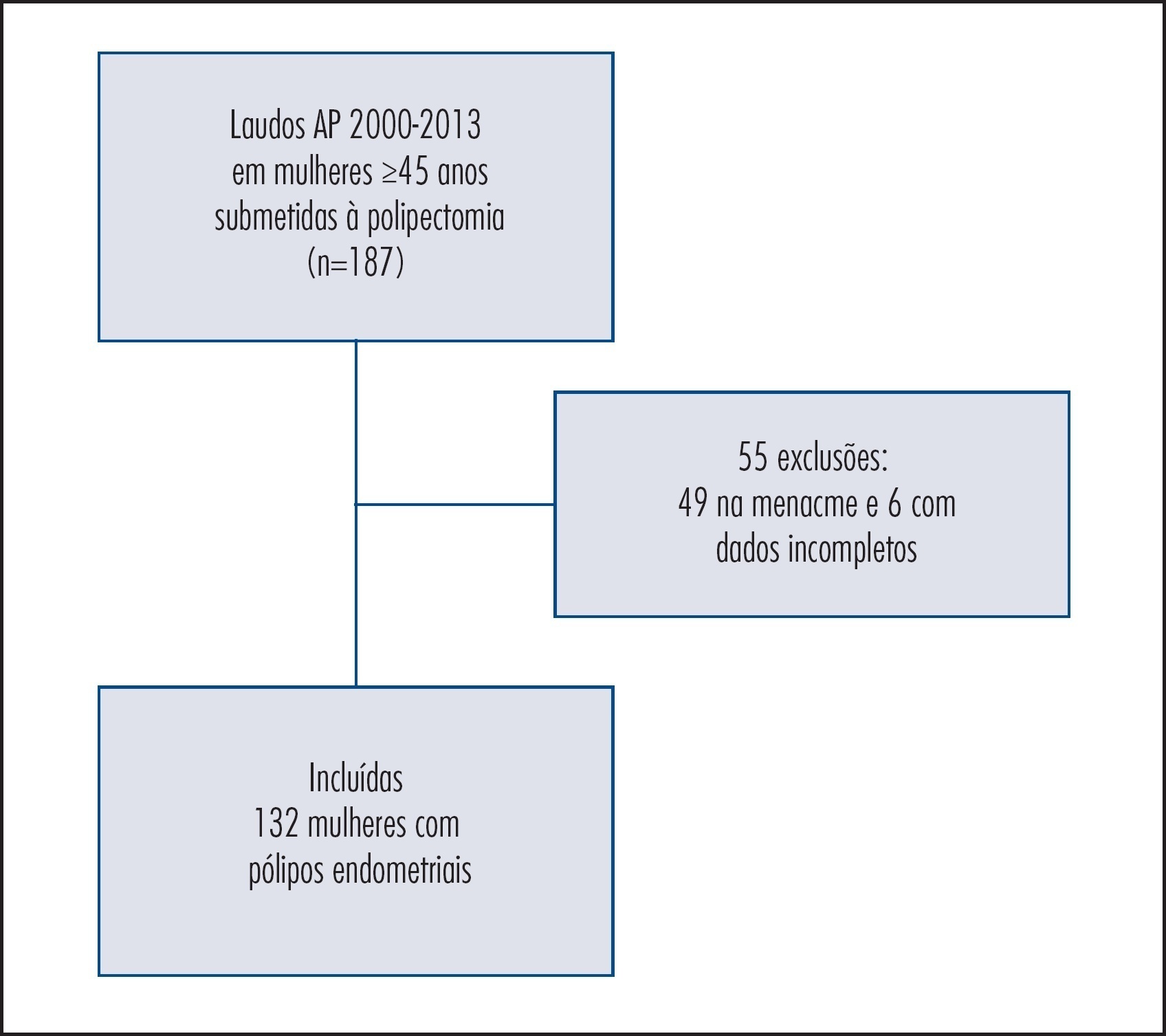
Observational cohort study with postmenopausal women who had been at a public university hospital. Clinical, anthropometrical, laboratorial, and ultrasonographic data of 132 patients with a histopathological diagnosis of endometrial polyps and 264 women without endometrial alterations (control) were compared in order to evaluate the predictive factors of endometrial polyps. Women with amenorrhea ≥12 months and ≥45 years of age were included in the study at a proportion of 1 case for 2 controls. The Student's t, χ2, and logistic regression tests were used for statistical analysis – odds ratio (OR).
Patients with endometrial polyps were older and had been in menopause for a longer time compared to control (p<0.0001). The percentage of obese women with polyps (72.0%) was higher compared to the Control Group (39%; p<0.0001). The measurement of waist circumference was superior among patients with polyps (p=0.0001). We observed a higher incidence of diabetes, hypertension and dyslipidemia in patients with endometrial polyps (p<0.0001). According to the US National Cholesterol Education Program/Adult Treatment Panel III (NCEP/ATP III) criteria, 48.5% of women with polyps and 33.3% of the Control Group were classified as having metabolic syndrome (p=0.004). Analysis of risk for endometrial polyps formation showed higher chances of occurrence of the disorder in patients with: BMI≥25 kg/m2 (OR=4.6; 95%CI 2.1–10.0); glucose ≥100 mg/dL (OR=2.8; 95%CI 1.3–5.9); dyslipidemia (OR=7.0; 95%CI 3.7–13.3); diabetes (OR=2.5; 95%CI 1.0–6.3), and metabolic syndrome (OR=2.7; 95%CI 1.1–6.4) compared to the Control Group.
In postmenopausal women, obesity, dyslipidemia, hyperglycemia and presence of metabolic syndrome were predictive factors for the development of endometrial polyps.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2014;36(11):489-496
DOI 10.1590/S0100-720320140005090
To evaluate the predictive clinical factors for the development of endometrial polyps in postmenopausal women.
Observational cohort study with postmenopausal women who had been at a public university hospital. Clinical, anthropometrical, laboratorial, and ultrasonographic data of 132 patients with a histopathological diagnosis of endometrial polyps and 264 women without endometrial alterations (control) were compared in order to evaluate the predictive factors of endometrial polyps. Women with amenorrhea ≥12 months and ≥45 years of age were included in the study at a proportion of 1 case for 2 controls. The Student's t, χ2, and logistic regression tests were used for statistical analysis – odds ratio (OR).
Patients with endometrial polyps were older and had been in menopause for a longer time compared to control (p<0.0001). The percentage of obese women with polyps (72.0%) was higher compared to the Control Group (39%; p<0.0001). The measurement of waist circumference was superior among patients with polyps (p=0.0001). We observed a higher incidence of diabetes, hypertension and dyslipidemia in patients with endometrial polyps (p<0.0001). According to the US National Cholesterol Education Program/Adult Treatment Panel III (NCEP/ATP III) criteria, 48.5% of women with polyps and 33.3% of the Control Group were classified as having metabolic syndrome (p=0.004). Analysis of risk for endometrial polyps formation showed higher chances of occurrence of the disorder in patients with: BMI≥25 kg/m2 (OR=4.6; 95%CI 2.1–10.0); glucose ≥100 mg/dL (OR=2.8; 95%CI 1.3–5.9); dyslipidemia (OR=7.0; 95%CI 3.7–13.3); diabetes (OR=2.5; 95%CI 1.0–6.3), and metabolic syndrome (OR=2.7; 95%CI 1.1–6.4) compared to the Control Group.
In postmenopausal women, obesity, dyslipidemia, hyperglycemia and presence of metabolic syndrome were predictive factors for the development of endometrial polyps.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2014;36(9):410-415
DOI 10.1590/SO100-720320140005078
To establish the prevalence of acanthosis nigricans (AN) within the context of polycystic ovary syndrome (PCOS) and its associations with obesity, insulin resistance, insulinemia, and metabolic syndrome (MS).
A cross-sectional prospective study was conducted on 100 patients with PCOS diagnosed according to the Rotterdam Consensus (2003). The skin test included, in addition to the detection of the presence of AN, the presence of hirsutism (score ≥8) and acne. In addition to clinical and biochemical data, we investigated cardiovascular risk factors present in MS such as abdominal circumference, obesity, hypertension and HDL and triglyceride levels. Insulin resistance was determined by the HOMA-IR test.
The prevalence of AN (53%) was significantly correlated with hirsutism (p=0.02), body mass index (p<0.01), basal insulinemia (p<0.01), (HOMA-IR) (p<0.01), and MS (p<0.01). The prevalence of MS reached 36% and was significantly associated only with AN (p<0.01). Although diabetes mellitus was absent, there was a significant association of altered HOMA-IR (p<0.01) with MS (p<5%) and AN (p<0.01).
AN is part of the severe phenotypic profile of PCOS as an additional predictable sign of the risks of cardiovascular disease.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2014;36(9):410-415
DOI 10.1590/SO100-720320140005078
To establish the prevalence of acanthosis nigricans (AN) within the context of polycystic ovary syndrome (PCOS) and its associations with obesity, insulin resistance, insulinemia, and metabolic syndrome (MS).
A cross-sectional prospective study was conducted on 100 patients with PCOS diagnosed according to the Rotterdam Consensus (2003). The skin test included, in addition to the detection of the presence of AN, the presence of hirsutism (score ≥8) and acne. In addition to clinical and biochemical data, we investigated cardiovascular risk factors present in MS such as abdominal circumference, obesity, hypertension and HDL and triglyceride levels. Insulin resistance was determined by the HOMA-IR test.
The prevalence of AN (53%) was significantly correlated with hirsutism (p=0.02), body mass index (p<0.01), basal insulinemia (p<0.01), (HOMA-IR) (p<0.01), and MS (p<0.01). The prevalence of MS reached 36% and was significantly associated only with AN (p<0.01). Although diabetes mellitus was absent, there was a significant association of altered HOMA-IR (p<0.01) with MS (p<5%) and AN (p<0.01).
AN is part of the severe phenotypic profile of PCOS as an additional predictable sign of the risks of cardiovascular disease.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(12):562-568
DOI 10.1590/S0100-72032013001200006
PURPOSE: To assess the contribution of hyperandrogenism to the development of metabolic syndrome (MetS) in obese women with polycystic ovary syndrome (PCOS). METHODS: Retrospective cross-sectional study conducted on 60 obese women with classic PCOS phenotype - Rotterdam Consensus - and 70 non-PCOS obese women. MetS was diagnosed by the NCEP-ATP III criteria and obesity was defined by body mass index. The Ferriman-Gallwey score (mFG) was used to evaluate hirsutism. The following measurements were performed: total testosterone, dehydroepiandrosterone sulfate (DHEA-S), glucose and insulin, total cholesterol, HDL, and triglycerides. Insulin resistance was measured using the HOMA-IR and insulin sensitivity index of Matsuda and De Fronzo (ISI). Statistical analysis was performed using the Student's t-test, χ² test and multivariate logistic regression analysis (p<0.05). RESULTS: Obese women with PCOS had significantly higher mFG (15.4±6.1), waist circunference (105.6±11.4 cm), DHEA-S (200.8±109.2 µg/dL), testosterone (135.8±71.4 ng/dL), and HOMA-IR (8.4±8.5) values and lower ISI values (2.0±1.8) than non-obese PCOS women (3.2±2.1; 101.4±9.2 cm; 155.0±92.7 µg/dL; 50.0±18.2 ng/dL; 5.1±4.7 and 3.3±2.7, respectively) (p<0.05). The frequency of MetS was higher in PCOS obese (75%) than non-PCOS obese (52.8%) women (p=0.015). Multivariate analysis did not reveal the contribution of the variables IFG, testosterone, and DHEAS to the development of MetS (p>0.05). CONCLUSION: Obese women with PCOS have a higher frequency of metabolic syndrome than non-PCOS obese women, and hyperandrogenism does not contribute to the development of metabolic syndrome in this group of women.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(12):562-568
DOI 10.1590/S0100-72032013001200006
PURPOSE: To assess the contribution of hyperandrogenism to the development of metabolic syndrome (MetS) in obese women with polycystic ovary syndrome (PCOS). METHODS: Retrospective cross-sectional study conducted on 60 obese women with classic PCOS phenotype - Rotterdam Consensus - and 70 non-PCOS obese women. MetS was diagnosed by the NCEP-ATP III criteria and obesity was defined by body mass index. The Ferriman-Gallwey score (mFG) was used to evaluate hirsutism. The following measurements were performed: total testosterone, dehydroepiandrosterone sulfate (DHEA-S), glucose and insulin, total cholesterol, HDL, and triglycerides. Insulin resistance was measured using the HOMA-IR and insulin sensitivity index of Matsuda and De Fronzo (ISI). Statistical analysis was performed using the Student's t-test, χ² test and multivariate logistic regression analysis (p<0.05). RESULTS: Obese women with PCOS had significantly higher mFG (15.4±6.1), waist circunference (105.6±11.4 cm), DHEA-S (200.8±109.2 µg/dL), testosterone (135.8±71.4 ng/dL), and HOMA-IR (8.4±8.5) values and lower ISI values (2.0±1.8) than non-obese PCOS women (3.2±2.1; 101.4±9.2 cm; 155.0±92.7 µg/dL; 50.0±18.2 ng/dL; 5.1±4.7 and 3.3±2.7, respectively) (p<0.05). The frequency of MetS was higher in PCOS obese (75%) than non-PCOS obese (52.8%) women (p=0.015). Multivariate analysis did not reveal the contribution of the variables IFG, testosterone, and DHEAS to the development of MetS (p>0.05). CONCLUSION: Obese women with PCOS have a higher frequency of metabolic syndrome than non-PCOS obese women, and hyperandrogenism does not contribute to the development of metabolic syndrome in this group of women.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(9):421-426
DOI 10.1590/S0100-72032013000900007
Polycystic ovary syndrome (PCOS) is an endocrine disorder associated with several cardiometabolic risk factors, such as central obesity, insulin resistance, type 2 diabetes, metabolic syndrome, and hypertension. These factors are associated with adrenergic overactivity, which is an important prognostic factor for the development of cardiovascular disorders. Given the common cardiometabolic disturbances occurring in PCOS women, over the last years studies have investigated the cardiac autonomic control of these patients, mainly based on heart rate variability (HRV). Thus, in this review, we will discuss the recent findings of the studies that investigated the HRV of women with PCOS, as well as noninvasive methods of analysis of autonomic control starting from basic indexes related to this methodology.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(9):421-426
DOI 10.1590/S0100-72032013000900007
Polycystic ovary syndrome (PCOS) is an endocrine disorder associated with several cardiometabolic risk factors, such as central obesity, insulin resistance, type 2 diabetes, metabolic syndrome, and hypertension. These factors are associated with adrenergic overactivity, which is an important prognostic factor for the development of cardiovascular disorders. Given the common cardiometabolic disturbances occurring in PCOS women, over the last years studies have investigated the cardiac autonomic control of these patients, mainly based on heart rate variability (HRV). Thus, in this review, we will discuss the recent findings of the studies that investigated the HRV of women with PCOS, as well as noninvasive methods of analysis of autonomic control starting from basic indexes related to this methodology.



Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(7):301-308
DOI 10.1590/S0100-72032013000700004
PURPOSE: To evaluate sexual function in postmenopausal women diagnosed with metabolic syndrome. METHODS: Case-control study with 195 postmenopausal women (amenorrhea ≥1 year, FSH≥30 mIU/mL, aged 43 to 69 years) seen at the Department of Obstetrics and Gynecology, School of Medical Sciences of Santa Casa de São Paulo and in the Basic Units of the Family Health Program of São Paulo. Clinical data were collected, and body mass index and waist circumference were evaluated. Total cholesterol, HDL and LDL cholesterols, triglycerides, and fasting glucose were determined for biochemical analysis. We considered women to have the metabolic syndrome when they met three or more diagnostic criteria: waist circumference>88 cm and triglycerides ≥150 mg/dL; cholesterol HDL <50 mg/dL; blood pressure ≥130/85 mmHg, and fasting glucose ≥110 mg/dL. The participants were divided into Control Group (n=87) and Metabolic Syndrome Group (n=108). The Female Sexual Function Index (FSFI) was employed to assess the sexual function. RESULTS: Mean age was 54.0±4.7 years. The rate of sexual dysfunction was significantly higher in women with the metabolic syndrome than in the Control Group, both when considering FSFI <26.5 (90/108 [83.3%] versus 42/87 [48.2%], p<0.0001) and FSFI <23 (62/108 [57.4%] versus 16/87 [18.39%], p<0.001). The domains desire, arousal, lubrication, orgasm (p<0.001), and satisfaction (p=0.002) had lower scores in women with the metabolic syndrome. For the pain scores, there was no significant difference (p=0.57) between groups. All components of the metabolic syndrome diagnosis were associated with higher levels of sexual dysfunction (p<0.001). CONCLUSION: Postmenopausal women with metabolic syndrome present more frequently sexual dysfunction than those of the same age who do not have it.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(7):301-308
DOI 10.1590/S0100-72032013000700004
PURPOSE: To evaluate sexual function in postmenopausal women diagnosed with metabolic syndrome. METHODS: Case-control study with 195 postmenopausal women (amenorrhea ≥1 year, FSH≥30 mIU/mL, aged 43 to 69 years) seen at the Department of Obstetrics and Gynecology, School of Medical Sciences of Santa Casa de São Paulo and in the Basic Units of the Family Health Program of São Paulo. Clinical data were collected, and body mass index and waist circumference were evaluated. Total cholesterol, HDL and LDL cholesterols, triglycerides, and fasting glucose were determined for biochemical analysis. We considered women to have the metabolic syndrome when they met three or more diagnostic criteria: waist circumference>88 cm and triglycerides ≥150 mg/dL; cholesterol HDL <50 mg/dL; blood pressure ≥130/85 mmHg, and fasting glucose ≥110 mg/dL. The participants were divided into Control Group (n=87) and Metabolic Syndrome Group (n=108). The Female Sexual Function Index (FSFI) was employed to assess the sexual function. RESULTS: Mean age was 54.0±4.7 years. The rate of sexual dysfunction was significantly higher in women with the metabolic syndrome than in the Control Group, both when considering FSFI <26.5 (90/108 [83.3%] versus 42/87 [48.2%], p<0.0001) and FSFI <23 (62/108 [57.4%] versus 16/87 [18.39%], p<0.001). The domains desire, arousal, lubrication, orgasm (p<0.001), and satisfaction (p=0.002) had lower scores in women with the metabolic syndrome. For the pain scores, there was no significant difference (p=0.57) between groups. All components of the metabolic syndrome diagnosis were associated with higher levels of sexual dysfunction (p<0.001). CONCLUSION: Postmenopausal women with metabolic syndrome present more frequently sexual dysfunction than those of the same age who do not have it.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(6):249-254
DOI 10.1590/S0100-72032013000600003
PURPOSE: To evaluate the clinical, ultrasonographic, biochemical and metabolic alterations of adolescents with polycystic ovary syndrome (PCOS). METHODS: Retrospective observational study conducted on 44 adolescents aged 12 to 19 years, diagnosed with PCOS according to the Rotterdam Consensus. Metabolic changes were assessed according to the recommendations of the International Diabetes Federation, considering: waist circumference (WC) >90th percentile (10-15 years of age) or >80 cm (age >16 years), fasting glucose >100 mg/dL, triglycerides >150 mg/dL, HDL <40 mg/dL, and blood pressure >Hg 130/85 mm. RESULTS: Mean age was 16.7±2.2 years and age at menarche was 11.8±1.4 years. The menstrual irregularity most frequently observed was amenorrhea (72.7%) followed by oligomenorrhea (27.3%); hirsutism was observed in 86.4% and acne in 56.8%. Polycystic ovaries were observed by ultrasound only in 27.3%. Mean BMI was 30.3±6.6 kg/m². According to BMI, 52.3% of adolescents were obese, 13.6% were overweight and 6.8% had a healthy weight. Increased waist circumference (63.6%, 28/44) and the reduction of HDL-C (34.1%, 15/44) were the metabolic changes most frequently observed. Increased triglycerides were observed in 27.3% (12/44) and increased blood pressure and impaired fasting glucose were found in 9.1% (4/44) and 4.5% (2/44) of cases, respectively. Acanthosis nigricans was observed in 52.3% and insulin resistance in 62.8% of the adolescents with PCOS. Metabolic syndrome was identified in six children (13.6%), all of them obese or overweight. CONCLUSION: In the adolescents with PCOS studied here, menstrual irregularity and hirsutism were the most common clinical manifestations, while the sonographic findings consistent with polycystic ovaries were less prevalent. Obesity associated with insulin resistance predisposes these adolescents to a higher frequency of metabolic disorders.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2013;35(6):249-254
DOI 10.1590/S0100-72032013000600003
PURPOSE: To evaluate the clinical, ultrasonographic, biochemical and metabolic alterations of adolescents with polycystic ovary syndrome (PCOS). METHODS: Retrospective observational study conducted on 44 adolescents aged 12 to 19 years, diagnosed with PCOS according to the Rotterdam Consensus. Metabolic changes were assessed according to the recommendations of the International Diabetes Federation, considering: waist circumference (WC) >90th percentile (10-15 years of age) or >80 cm (age >16 years), fasting glucose >100 mg/dL, triglycerides >150 mg/dL, HDL <40 mg/dL, and blood pressure >Hg 130/85 mm. RESULTS: Mean age was 16.7±2.2 years and age at menarche was 11.8±1.4 years. The menstrual irregularity most frequently observed was amenorrhea (72.7%) followed by oligomenorrhea (27.3%); hirsutism was observed in 86.4% and acne in 56.8%. Polycystic ovaries were observed by ultrasound only in 27.3%. Mean BMI was 30.3±6.6 kg/m². According to BMI, 52.3% of adolescents were obese, 13.6% were overweight and 6.8% had a healthy weight. Increased waist circumference (63.6%, 28/44) and the reduction of HDL-C (34.1%, 15/44) were the metabolic changes most frequently observed. Increased triglycerides were observed in 27.3% (12/44) and increased blood pressure and impaired fasting glucose were found in 9.1% (4/44) and 4.5% (2/44) of cases, respectively. Acanthosis nigricans was observed in 52.3% and insulin resistance in 62.8% of the adolescents with PCOS. Metabolic syndrome was identified in six children (13.6%), all of them obese or overweight. CONCLUSION: In the adolescents with PCOS studied here, menstrual irregularity and hirsutism were the most common clinical manifestations, while the sonographic findings consistent with polycystic ovaries were less prevalent. Obesity associated with insulin resistance predisposes these adolescents to a higher frequency of metabolic disorders.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(12):555-562
DOI 10.1590/S0100-72032012001200005
PURPOSE: To assess the occurrence of metabolic syndrome (MetS) in postmenopausal breast cancer survivors. METHODS: A total of 158 breast cancer survivors were included in this cross-sectional study. Eligibility criteria were: women with amenorrhea >12 months and age ≥45 years, treated for breast cancer and no metastasis for at least five years. Clinical history and anthropometric indicator data (body mass index (BMI), and waist circumference, (WC) were collected. Biochemical parameters, including total cholesterol, HDL, LDL, triglycerides (TG), glucose and C-reactive protein (CRP), were measured. MetS was diagnosed as the presence of at least three of the following diagnostic criteria: WC>88 cm, blood pressure≥130/85 mmHg, triglycerides≥150 mg/dl, HDL <50 mg/dL,and glucose≥100 mg/dL. The Student's t-test and χ² test were used for statistical analysis. RESULTS: The mean age of breast cancer survivors was 63.1±8.6 years, with a mean follow-up of 9.1±4.0 years. MetS was diagnosed in 48.1% (76/158) and the most prevalent diagnostic criterion was abdominal obesity (WC>88 cm), affecting 54.4% (86/158) of the women. The patients without MetS had a longer follow-up compared those with MetS (p<0.05). Regarding the current BMI, PN average, those without MetS were overweight, and those with MetS were obese (p<0.05). Among the latter, comparison of BMI at the time of cancer diagnosis and current BMI (27.8±5.4 versus 33.4±5.4 kg/m²) showed a significant weight gain (p<0.05). Mean CRP values were higher in women with MetS (p<0.05). In the comparison of tumor characteristics and cancer treatments there was no difference between groups (p>0.05). CONCLUSION: Postmenopausal breast cancer survivors had a higher risk of developing metabolic syndrome and central obesity.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(12):555-562
DOI 10.1590/S0100-72032012001200005
PURPOSE: To assess the occurrence of metabolic syndrome (MetS) in postmenopausal breast cancer survivors. METHODS: A total of 158 breast cancer survivors were included in this cross-sectional study. Eligibility criteria were: women with amenorrhea >12 months and age ≥45 years, treated for breast cancer and no metastasis for at least five years. Clinical history and anthropometric indicator data (body mass index (BMI), and waist circumference, (WC) were collected. Biochemical parameters, including total cholesterol, HDL, LDL, triglycerides (TG), glucose and C-reactive protein (CRP), were measured. MetS was diagnosed as the presence of at least three of the following diagnostic criteria: WC>88 cm, blood pressure≥130/85 mmHg, triglycerides≥150 mg/dl, HDL <50 mg/dL,and glucose≥100 mg/dL. The Student's t-test and χ² test were used for statistical analysis. RESULTS: The mean age of breast cancer survivors was 63.1±8.6 years, with a mean follow-up of 9.1±4.0 years. MetS was diagnosed in 48.1% (76/158) and the most prevalent diagnostic criterion was abdominal obesity (WC>88 cm), affecting 54.4% (86/158) of the women. The patients without MetS had a longer follow-up compared those with MetS (p<0.05). Regarding the current BMI, PN average, those without MetS were overweight, and those with MetS were obese (p<0.05). Among the latter, comparison of BMI at the time of cancer diagnosis and current BMI (27.8±5.4 versus 33.4±5.4 kg/m²) showed a significant weight gain (p<0.05). Mean CRP values were higher in women with MetS (p<0.05). In the comparison of tumor characteristics and cancer treatments there was no difference between groups (p>0.05). CONCLUSION: Postmenopausal breast cancer survivors had a higher risk of developing metabolic syndrome and central obesity.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(8):357-361
DOI 10.1590/S0100-72032012000800003
PURPOSE: To compare the frequency of metabolic syndrome (MetS) and the risk factors associated with this syndrome in women from the Brazilian Southeast with polycystic ovary syndrome (POS) evaluated during adolescence and adult age. METHODS: This was a cross-sectional study conducted on 147 patients with a diagnosis of POS who were divided into two groups: Adolescents, 42 adolescents aged 13 to 19 years, and Adults, 105 women aged 20 to 40 years. The following factors were evaluated: clinical characteristics (body mass index - BMI, Ferriman index, abdominal circumference - AC, and systemic arterial pressure), mean ovarian volume, laboratory variables (serum androgen profile, lipid profile, glycemia, and fasting insulin), and frequency of MetS. The results were expressed as mean±standard deviation. We used multiple logistic regression with the response variable being the presence of MetS and the predictor variables the levels of total testosterone, insulin and BMI. RESULTS: The frequency of MetS was approximately twice higher in the group of adult women compared to the adolescents with POS (Adolescents: 23.8 vs. Adults: 42.9%, p=0.04). Among the defining criteria of MetS, only the qualitative variable of systemic arterial pressure ≥130/85 mmHg was more frequent among the adult women (p=0,01). The BMI was an independent predictor of MetS among the adolescent (p=0.03) and adult women (p<0.01) with POS. Serum insulin level was a predictor of MetS only among adult women with POS (p<0.01). AC was greater among adult women (p=0.04). CONCLUSION: Adult women with POS have a twice higher frequency of MetS than adolescents with POS from the Brazilian Southeast. Although the BMI is associated with the development of MetS in any phase of life in women with POS, serum insulin level was an independent predictor of MetS only among adult women with this disorder.


Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2012;34(8):357-361
DOI 10.1590/S0100-72032012000800003
PURPOSE: To compare the frequency of metabolic syndrome (MetS) and the risk factors associated with this syndrome in women from the Brazilian Southeast with polycystic ovary syndrome (POS) evaluated during adolescence and adult age. METHODS: This was a cross-sectional study conducted on 147 patients with a diagnosis of POS who were divided into two groups: Adolescents, 42 adolescents aged 13 to 19 years, and Adults, 105 women aged 20 to 40 years. The following factors were evaluated: clinical characteristics (body mass index - BMI, Ferriman index, abdominal circumference - AC, and systemic arterial pressure), mean ovarian volume, laboratory variables (serum androgen profile, lipid profile, glycemia, and fasting insulin), and frequency of MetS. The results were expressed as mean±standard deviation. We used multiple logistic regression with the response variable being the presence of MetS and the predictor variables the levels of total testosterone, insulin and BMI. RESULTS: The frequency of MetS was approximately twice higher in the group of adult women compared to the adolescents with POS (Adolescents: 23.8 vs. Adults: 42.9%, p=0.04). Among the defining criteria of MetS, only the qualitative variable of systemic arterial pressure ≥130/85 mmHg was more frequent among the adult women (p=0,01). The BMI was an independent predictor of MetS among the adolescent (p=0.03) and adult women (p<0.01) with POS. Serum insulin level was a predictor of MetS only among adult women with POS (p<0.01). AC was greater among adult women (p=0.04). CONCLUSION: Adult women with POS have a twice higher frequency of MetS than adolescents with POS from the Brazilian Southeast. Although the BMI is associated with the development of MetS in any phase of life in women with POS, serum insulin level was an independent predictor of MetS only among adult women with this disorder.


Search
Search in:
breast breast cancer Breast neoplasms Cesarean section Endometriosis infertility Maternal mortality Menopause Obesity Polycystic ovary syndrome Postpartum period Pregnancy Pregnancy complications Prenatal care prenatal diagnosis Quality of life Risk factors Ultrasonography Uterine cervical neoplasms Women’s health
