Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(7):435-436
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(7):434-434
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(7):434-434
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(7):435-435
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(7):436-436
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(6):353-356
DOI 10.1590/S0100-72032005000600010
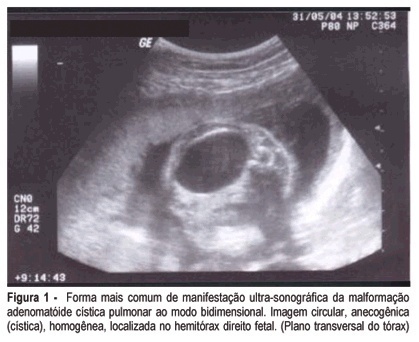
Fetal cystic adenomatoid malformation is a pulmonary developmental anomaly arising from an overgrowth of the terminal respiratory bronchioles. This is such a rare malformation, that is not always thought of as a diagnostic possibility. We present a case of pulmonary cystic adenomatoid malformation and emphasize the importance of early diagnosis and therapeutic possibilities. We also present its evolution after prenatal placement of a catheter for continuous drainage.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(7):373-375
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(7):382-386
DOI 10.1590/S0100-72032005000700003
PURPOSE: to evaluate periodontal conditions and need for treatment supplied by Periodontal Screening and Recording (PSR) in mothers, in order to clarify the relationship between periodontal disease and low birth weight premature newborns. METHODS: PSR was used in a sample of 40 mothers, divided into: test group, consisting of mothers of premature newborns with weight less than 2,500 g (n=20), and the control group, consisting of mothers of term newborns with a weight equal to or over 2,500 g (n=20). The collected data were analyzed by descriptive statistics, and the results of PSR were submitted to statistical analysis in order to verify differences in periodontal condition and need for treatment of the mothers, using the Kolmogorov-Smirnov test, with a significance level of 5%. RESULTS: the presence of periodontal pocket of 3.5 to 5.5 mm was the most common finding among the mothers of newborns with low weight (39.2% of the cases), while the presence of bleeding at probing and absence of a periodontal pocket were the most frequent findings among the mothers of newborns with normal weight (37.5% of the cases). There was a statistically significant difference between periodontal conditions of the mothers of the groups (p=0.0494), but in relation to the need for treatment, there was no significant difference between the studied groups (p>0.05). CONCLUSION: the mothers of preterm newborns with low weight presented worse periodontal conditions, suggesting that periodontal infection may be related to preterm low birth weight newborns.