You searched for:"Marcos Dias de Moura"
We found (12) results for your search.Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(1):31-35
DOI 10.1590/S0100-72032008000100006
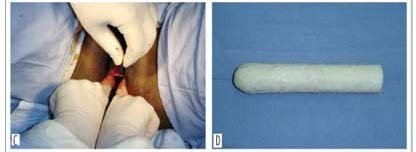
PURPOSE: to evaluate the use of natural latex mold (Hevea brasiliensis) as a modification of McIndoe and Bannister neovaginoplasty in patients presenting Mayer-Rokitansky-Küster-Hauser (MKRH) syndrome. METHODS: we retrospectively included nine patients presenting MKRH syndrome, who had been submitted to McIndoe and Bannister neovaginoplasty modified by the use of natural latex mold. Neovaginal epithelization and depth, coitus occurrence and satisfaction, and surgical complications were evaluated. RESULTS: five weeks after the procedure, eight patients presented an epithelized 7 to 12 cm deep neovagina. There was one case of complete neovaginal stenosis, because of incorrect use of the mold. After at least one year, the others maintained 4 to 8 cm deep neovaginas and capacity for intercourse, with 66.7% satisfaction. One woman presented precocious rectovaginal fistula and late episodes of uretrovaginal fistulae. Two patients presented distal neovaginal stenosis in long-term follow-up. One of these and the patient with fistulae were submitted to a new procedure. CONCLUSIONS: the use of natural latex mold as a modification of classic neovaginoplasty technique allows the creation of neovaginas morphologically and functionally similar to the normal vagina in patients with vaginal agenesis.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(12):619-624
DOI 10.1590/S0100-72032007001200004
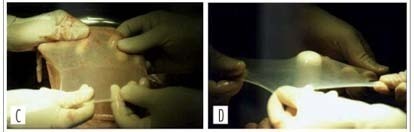
PURPOSE: to evaluate the results of neovaginoplasty with the use of a human amniotic graft in patients with the Mayer-Rokitansky-Küster-Hauser (MRKH) syndrome. METHODS: the study was a retrospective analysis of a series of 28 patients with the MRKH syndrome conducted from 1990 to 2003. The patients were attended and treated at the Ambulatório de Ginecologia Infanto-Puberal (AGIP) of the Hospital Universitário of the Faculdade de Medicina de Ribeirão Preto of the Universidade de São Paulo (FMRP-USP), being submitted to neovaginoplasty by the technique of McIndoe and Bannister, modified by the use of a human amniotic membrane graft. Epithelization, amplitude and depth of the neovaginas were evaluated 7 and 40 days after the procedure. Patient satisfaction was determined during the late postoperative period in terms of the presence of discomfort and dyspareunia during sexual relations. RESULTS: postoperatively, seven patients (25%) presented vaginal stenosis and six of them were submitted to a new surgical intervention, one had shortening of the neovagina, corrected with the use of exercises with a vaginal mold, three (10.7%) developed a rectovaginal fistula, one (3.6%) a uterovesical fistula, and one (3.6%) excess skin in the vaginal introitus - all successfully corrected with surgery. Four patients (14.3%) presented urinary tract infection. Two months after surgery, 11/19 patients (57.8%) presented satisfactory sexual activity and 42% dyspareunia, and within a maximum period of four years, 20/21 patients (95.2%) had satisfactory sexual activity and 4.8% dyspareunia. CONCLUSIONS: an amniotic membrane graft is a good option for the treatment of vaginal agenesis. Perioperative follow-up involves educational guidance regarding the use of the mold and regarding patient sexuality in order to reduce the complaints of dysfunctional coitus in the presence of a favorable surgical evolution and a neovagina of adequate aspect.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2007;29(6):303-309
DOI 10.1590/S0100-72032007000600005
PURPOSE: to assess the level of lipid peroxidation (LP) and vitamin E in the follicular fluid and serum of infertile patients, with or without endometriosis, submitted to induction of ovulation for assisted reproduction procedures. METHODS: infertile patients aged 20 to 38 years old were selected prospectively and consecutively and divided into Endometriosis Group (17 patients with pelvic endometriosis) and Control Group (19 patients with previous tubal ligation or with male factor). Blood samples were collected on: D1 (before the beginning of the use of gonadotrophins), D2 (day of human chorionic gonadotrofin application) and D3 (day of oocyte retrieval). On D3, follicular fluid samples free from blood contamination were also collected and stored. LP was assessed for malondialdehyde (MDA) quantification by spectrophotometry, and antioxidant status by measurement of vitamin E by HLPC. RESULTS: on D1, no significant difference in LP was observed between groups. However, vitamin E levels were significantly higher in the Control Group. On D2, LP levels were significantly higher in the Endometriosis Group compared to Control and vitamin E levels continued to be significantly higher in the Control Group. On D3, there was no significant difference in both serum and follicular fluid levels of LP or vitamin E between groups. However, on D3, vitamin E levels were found to be significantly higher in serum than in follicular fluid in both groups, whereas MDA levels were significantly lower in follicular fluid than in serum only in the Control Group. CONCLUSION: before the beginning of the induction of ovulation, a significant decrease in antioxidant status was observed in patients with endometriosis, perhaps because antioxidants are consumed during oxidation reactions. After the induction of ovulation with exogenous gonadotrophins, the group of patients with endometriosis presented not only increased lipid peroxidation compared to Control, but also maintained a lower antioxidant status than the Control Group. However, on the day of oocyte retrieval, both serum LP potential and the levels of vitamin E were found to be similar in both groups.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1999;21(2):85-90
DOI 10.1590/S0100-72031999000200005
Purpose: to present a profile of endometriosis, stages and results of treatment among the patients seen in our Service. Methods: the medical records of 155 patients with endometriosis treated during the period from 1991 to 1996 according to a preestablished protocol were examined. Results: mean patient age was 31 years, most patients were white, with regular menstrual cycles. The most frequently observed symptoms were dysmenorrhea, pelvic pain and infertility and were mild in most of the cases. The diagnostic methods utilized were laparoscopy or echography. There was agreement between echography and laparoscopy in 96% of cases. Laparotomy was required in 28% of cases for diagnostic elucidation and/or treatment. Endometrioma was detected in 37% of the cases and endometriosis was confirmed in only 74% of the biopsies from the lesion by anatomopathological examination. There was a significant improvement with clinical treatment regardless of the drug used, with improved symptoms in approximately 50% of the patients. Assisted fertilization was performed in 34 patients, consisting of in vitro fertilization (IVF) for 80% of them, with a 27% pregnancy/transfer rate. Conclusions: the diagnostic method of choice should be laparoscopy, although echography presented a high rate of agreement. Anatomopathological examination of the lesions should be used as an adjuvant method in the diagnosis since it is not confirmatory in all of the cases. Clinical treatment with assisted reproductive technologies is a good therapeutic option, especially with the use of IVF.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(11):643-651
DOI 10.1590/S0100-72032006001100003
PURPOSE: literature reports show that there are no conclusive data about the association between endometriosis and the concentrations of hormones involved in the control of reproduction. Thus, the present study was undertaken to determine FSH, LH, estradiol (E), progesterone (P), and histamine (Hi) concentrations in serum, peritoneal fluid and follicular fluid of women with and without endometriosis. METHODS: the extent of the disease was staged according to the revised American Fertility Society classification (1997). For the collection of serum and peritoneal fluid, 28 women with endometriosis undergoing diagnostic laparoscopy were selected (18 infertile women with endometriosis I-II and ten infertile women with endometriosis III-IV). For the control group, 21 fertile women undergoing laparoscopy for tubal sterilization were selected. Follicular fluid was obtained from 39 infertile women undergoing in vitro fertilization (21 women with endometriosis and 18 women without endometriosis). RESULTS: FSH and LH levels in serum, peritoneal fluid and follicular fluid did not differ significantly between groups. On the other hand, E and P concentrations in the peritoneal fluid were significantly lower in infertile women with endometriosis (E: 154.2±15.3 for stages I-II and 89.3 ng/mL±9.8 ng/mL for stages III-IV; P: 11.2±1.5 for stages I-II and 7.6 ng/mL±0.8 for stages III-IV) in comparison with control women (E: 289.1 ng/mL±30.1; P: 32.8±4.1 ng/mL) (Kruskal-Wallis/Dunn tests; p<0.05). In serum, estradiol and progesterone concentrations followed the same pattern. In the follicular fluid, E and Hi concentrations were significantly lower in women with endometriosis (E: 97.4±11.1 pg/mL; Hi: 6.6±0.9 ng/mL) in comparison to women without endometriosis (E: 237.5±28.5 pg/mL; Hi: 13.8±1.3 ng/mL) (Student t-test; p<0.05), while progesterone levels revealed no significant difference between groups. CONCLUSIONS: our results indicate ovary dysfunction in women with endometriosis, with reduction on E, P and Hi concentrations, which may contribute to the subfertility often associated with the disease.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(1):32-37
DOI 10.1590/S0100-72032006000100006
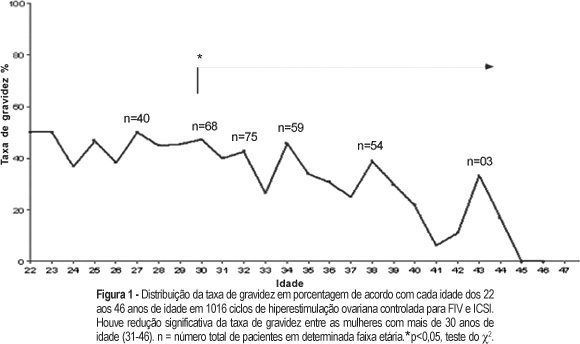
PURPOSE: to evaluate the rate of chemically diagnosed pregnancy (serum beta-HCG>25 mIU/mL levels obtained fourteen days after the embryonic transfer) clinically diagnosed pregnancy (gestational sac visualized by ultrasound four to six weeks after the embryonic transfer) and miscarriage rates in women submitted in vitro fertilization to (IVF) and intracytoplasmic sperm injection (ICSI) in a tertiary center of assisted reproduction and to correlate these rates with age. METHODS: retrospective transverse study with analysis of 1016 cycles of controlled ovarian hyperstimulation of 932 infertile women with indication of IVF (370 cycles) or ICSI (646 cycles). The patients' age ranged from 22 to 46 years. All women with age over 35 years included in the study had FSH<15 IU/L. The studied cycles were divided into two groups: the first including the cycles referring to women of 22 to 30 years and the second group, to those of 31 to 46 years. The studied variables were: pregnancy (chemical or clinical) and miscarriage rates. The chi2 test was used to compare these rates between the groups. RESULTS: the total pregnancy rate was 36.42%, with a significant reduction starting at 30 years (p=0.0001). From 22 to 30 years (303 cycles) the pregnancy rate was 45.4%, while in the range from 31 to 46 years (713 cycles), it was 25.1%. The miscarriage rates were, 10.2 11,6%, respectively (p=0.6854). CONCLUSION: although the miscarriage rates did not differ between the groups, a decrease in the pregnancy rate of infertile women submitted to IVF or ICSI was observed after the age of 30 years. Thus, we recommend the gynecologists not to postpone the investigation and the referral for treatment of infertility.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(9):529-533
DOI 10.1590/S0100-72032005000900005
PURPOSE: to study the histological modifications that occur in the endometrium of women before and six months after tubal ligation (TL) and to correlate these findings with progesterone (P4) levels. METHODS: the study was conducted on 16 women with normal menstrual cycles who were evaluated before and in the sixth cycle after TL. P4 levels were determined from the 8th day at 2-day intervals until ovulation and on the 8th, 10th and 12th day after ovulation or on the 24th day of the cycle. An endometrial biopsy was obtained between the 10th and 12th day after ovulation or on the 24th day of the cycle and a correlation with P4 was determined. Data were analyzed statistically by the nonparametric McNemar test for the evaluation of hormonal determination and by the exact Fisher test for the histological evaluation of the endometrium, with the level of significance set at p<0.05. RESULTS: mean age was 34.1±1.3 years. The intermenstrual interval was 27.1±2.6 days and the duration of bleeding was 3 to 5 days, with no difference between the studied periods. Before TL, 8/16 (50.0%) of the cases had a secretory endometrium according to the cycle, 3/16 (18.8%) had a secretory endometrium not according to the cycle and 3/16 (18.8%) had a dysfunctional endometrium, suggesting a defect in the luteal phase in 6/16 (37.5%). After TL, 7/16 (43.8%) had a secretory endometrium according to the cycle, 3/16 (18.8%) a secretory endometrium not according to the cycle and 4/16 (25.0%) had a dysfunctional endometrium, suggesting a defect in the luteal phase in 7/16 (43.8%). In 2/16 (12.5%) of the cases before TL and in 2/16 (12.5%) other cases after TL it was not possible to perform histological evaluation due to insufficient material or unspecfiic endometritis. In the luteal phase after TL, mean P4 levels were significantly lower on days +8, +10 and +12 than before TL, being 15.1, 18.0 and 20.7 ng/ml, respectively, before TL and 10.6, 8.0 and 5.4 ng/ml after TL (p<0.05). Before TL, 5/8 (62.5%) of the cases with a secretory endometrium according to the cycle had P4 >10 ng/ml and 3/8 (37.5%) had P4 <10 ng/ml. After TL, when the endometrium was secretory according to the cycle, P4 was >10 ng/ml in 4/7 (57.1%) and <10 ng/ml in 3/7 (42.9%). These differences were nonsignificant (p>0.05). CONCLUSION: six months after TL, the intermenstrual interval and the duration of bleeding were unchanged. P4 levels decreased during the luteal phase although this did not interfere in the endometrial response.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(2):89-94
DOI 10.1590/S0100-72032000000200005
Purpose: to evaluate the lipid profile (cholesterol, triglycerides, HDL and LDL) of women with polycystic ovary syndrome (PCO) and compare it to that of women with ovulatory menstrual cycles. Methods: the patients were divided into two groups, obese and nonobese, based on body mass index, so that it would be possible to determine the joint effect of PCO and obesity on the lipid metabolism of the studied women. We studied 117 women divided into 4 groups: group I (PCO--obese), n = 33; group II (PCO--nonobese), n = 27; group III (control--obese), n = 28; group IV (control--nonobese), n = 29. Results: cholesterol levels were elevated (179 mg/dl) in obese patients with ovulatory cycles (group III) compared to group I (147 mg/dl) and group II (149 mg/dl), as also were triglyceride levels (117 mg/dl) compared to group IV (77 mg/dl) and LDL levels (117 mg/dl) compared to group I (82 mg/dl). Conclusion: these data suggest that alterations in lipid profile are related to obesity only.