Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2010;32(2):82-87
DOI 10.1590/S0100-72032010000200006
PURPOSE: to study the clinical and microbiological profile of women with bacterial vaginosis participating in a randomized, double-blind clinical trial, which compared the vaginal use of preparations from red pepper tree and metronidazole for the treatment of genital discharge. METHODS: the study was conducted on a series of 277 women with bacterial vaginosis concomitantly diagnosed by the criteria of Amsel and Nugent, selected from a total of 462 recruited patients using the information obtained before intervention. Data were analyzed with the Epi-Info 3.32 software. In order to compare the outcomes frequencies between the intervention groups, the χ2 test was used and the risk ratio and 95% confidence interval were calculated. The intention to treat analysis was performed. In addition to the determination of diagnostic parameters, the culture of vaginal content and a Papanicolaou cytology test were also performed. RESULTS: the most frequent clinical complaints were genital discharge, observed in 206 participants (74.4%) and the fish odor of the vaginal secretion, which occurred in 68.6% of the cases (190 patients). Among the diagnostic clinical criteria, the presence of clue-cells was positive in 275 women (99.3%), the Whiff test, in 266 (96.0%), followed by pH >4.5, which occurred in 92.8% of the cases, and by the presence of fluid grayish discharge reported by 206 participants (74.4%). Regarding the Nugent criterion, the median score was 8.0. Culture of the vaginal content permitted the identification of Gardnerella vaginalis in 96.8% of cases and of Mobiluncus in 53.1%. Only one third of the exams showed the presence of Lactobacillus (89 women - 32.1%). Fungal growth occurred in the cultures of 14 participants (5.1%). In most cases, culture revealed the presence of Corynebacterium (94.2%), Gram-positive cocci (98.2%), as well as Gram-positive (99.3%) and Gram-negative (91.0%) bacilli. Oncotic colposcopy revealed a very scarce presence of lactobacilli, which were present in only 8 cytological exams (2.9%) out of the total of 273 exams performed. CONCLUSIONS: the results of the present study did not differ from the literature regarding the symptoms reported by the women, the clinical criteria most frequently observed in the diagnosis, or the bacterial species detected in cultures of vaginal content. These findings indicate the need for further studies that might better elucidate the interrelations between the microbiological findings and the clinical expression of bacterial vaginosis.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2021;43(11):820-825
To compare maternal and perinatal risk factors associated with complete uterine rupture and uterine dehiscence.
Cross-sectional study of patients with uterine rupture/dehiscence from January 1998 to December 2017 (30 years) admitted at the Labor and Delivery Unit of a tertiary teaching hospital in Canada.
There were 174 (0.1%) cases of uterine disruption (29 ruptures and 145 cases of dehiscence) out of 169,356 deliveries. There were associations between dehiscence and multiparity (odds ratio [OR]: 3.2; p=0.02), elevated maternal body mass index (BMI; OR: 3.4; p=0.02), attempt of vaginal birth after a cesarian section (OR: 2.9; p=0.05) and 5-minute low Apgar score (OR: 5.9; p<0.001). Uterine rupture was associated with preterm deliveries (36.5 ± 4.9 versus 38.2 ± 2.9; p=0.006), postpartum hemorrhage (OR: 13.9; p<0.001), hysterectomy (OR: 23.0; p=0.002), and stillbirth (OR: 8.2; p<0.001). There were no associations between uterine rupture and maternal age, gestational age, onset of labor, spontaneous or artificial rupture of membranes, use of oxytocin, type of uterine incision, and birthweight.
This large cohort demonstrated that there are different risk factors associated with either uterine rupture or dehiscence. Uterine rupture still represents a great threat to fetal-maternal health and, differently from the common belief, uterine dehiscence can also compromise perinatal outcomes.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(12):820-828
To evaluate the distribution of the main sociodemographic and clinicalpathological characteristics in women with breast cancer according to the molecular profile by immunohistochemistry.
A cross-sectional, retrospective, analytical and quantitative study was performed, with an analysis of 137 medical records from January 2015 to December 2018 of women attending the High Complexity in Oncology Unit of the city of Imperatriz, state of Maranhão, Brazil. The immunohistochemical profile of tumors based on the estrogen and progesterone receptor, Human Epidermal growth factor Receptor-type 2 (HER2) overexpression and Ki67 cell proliferation indexwas defined, fromwhich six molecular subtypes were determined: luminal A, luminal B-HER2 negative, luminal B-HER2 positive, triple negative, overexpression of HER2 and inconclusive.
A total of 52.6% of the patients were postmenopausal, mean age 52.1 years old, brown (56.2%), had a schooling level < 9 years (40%), staging > IIB (52.6%) and 23.4% hadmetastasis. Invasive ductal carcinoma accounted for 84.7%, tumor size was 2 to 5 cm (48.9%), with lymph node involvement (56.2%), axillary lymphadenectomy in 67.2%, andmastectomy in 73.7% of the patients. Themost frequentmolecular subtype was the luminal B-HER2 negative (36.5%), and the luminal A subtype showed characteristics of better prognosis when compared with the others.
It was concluded that in the association of molecular subtypes with sociodemographic and clinical-pathological characteristics, there were no statistically significant results obtained, except for complementary therapy, referring to hormone therapy, and there was a high index of metastasis at diagnosis, which was a worrying factor and indicative of failures in the screening and early diagnosis of this population.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(9):821-829
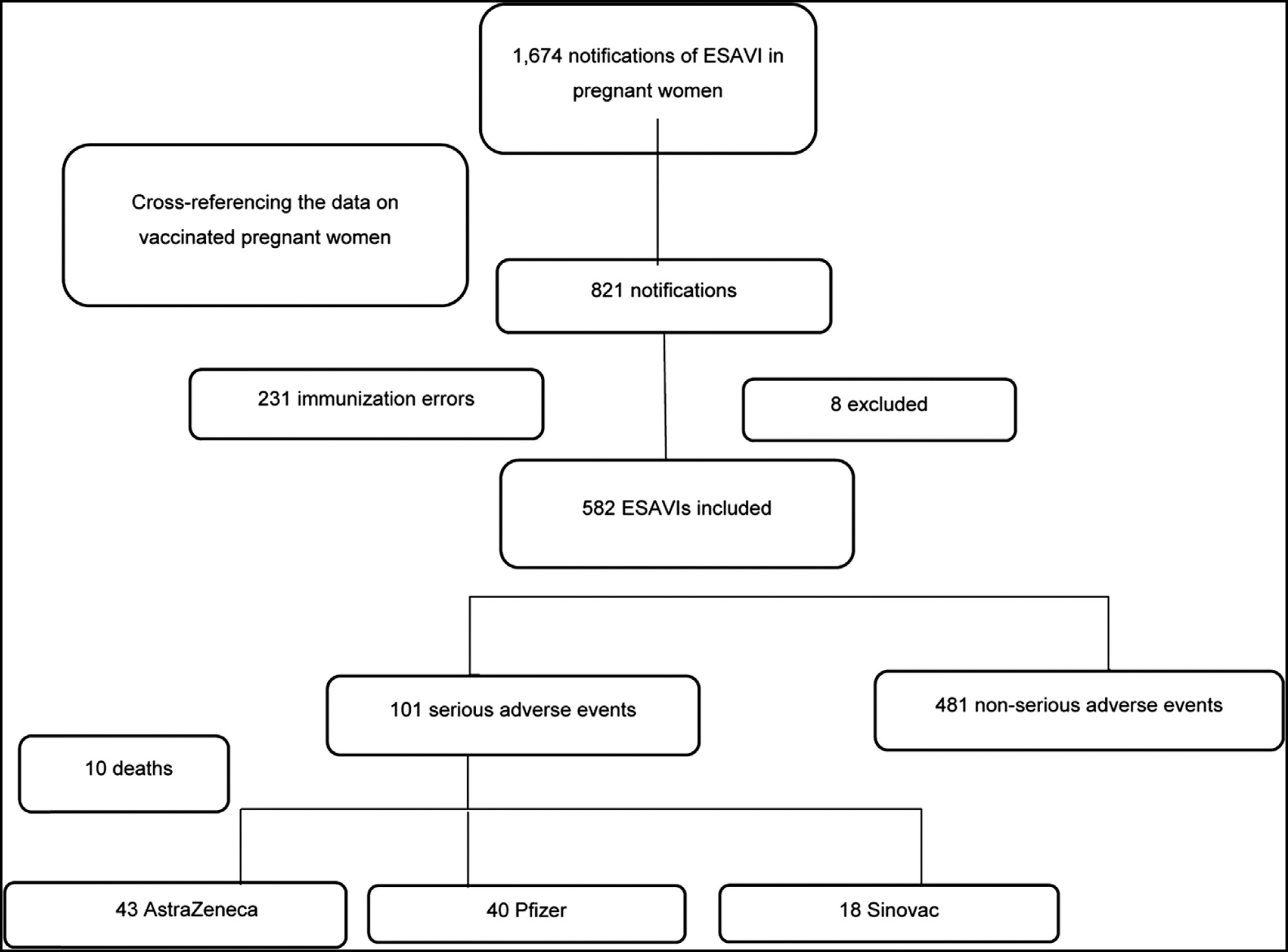
Regulations for the vaccination of pregnant women in Brazil occurred in March 2021. Despite the absence of robust data in the literature on the coronavirus disease 2019 (COVID-19) vaccinations in pregnant women, it is understood that the benefit-risk ratio tends to be favorable when considering the pandemic and the high burden of the disease. However, it is still important to monitor for Events Supposedly Attributable to Vaccination or Immunization (ESAVI) and to draw safety profiles of the different platforms used in pregnant and postpartum women. The present study aims to describe the main characteristics of ESAVIs related to COVID-19 vaccines occurring in pregnant women in the first months of the vaccination campaign in Brazil. During the evaluation period, 1,674 notifications of ESAVIs in pregnant women were recorded, and 582 notifications were included for the analysis. Of the 582 ESAVIs identified, 481 (82%) were classified as non-serious adverse events and 101 (17%) as serious adverse events. Ten deaths were identified, including one death which was considered to be causally related to the vaccine. The other nine maternal deaths had causality C, that is, without causal relationship with the vaccine, and most were due to complications inherent to pregnancy, such as pregnancy-specific hypertensive disorder (PSHD) in 4 cases and 3 due to COVID-19. Despite some limitations in our study, we believe it brings new insights into COVID-19 vaccines in this group and will add to the available evidence.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(12):829-833
Thyroid diseases are relatively common in women in the reproductive period. It is currently understood that clinically-evident thyroid disorders may impair ovulation and, consequently, fertility. However, to date it has not been proven that high serum levels of thyroid-stimulating hormone and/or positivity for antithyroid antibodies are associated to a reduction in fertility, mainly in the absence of altered thyroxine levels. The present comprehensive review aims to present current data on the association between subclinical hypothyroidism and/or thyroid autoimmunity and reproductive outcomes.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(1):83-88
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 1998;20(2):83-89
DOI 10.1590/S0100-72031998000200005
Results on investigation and immune treatment for recurrent abortion are presented. Up to 60% of patients who are free of any clinical identifiable cause for abortion are believed to have alloimmune abnormalities. One of the suggested therapies for this condition is paternal lymphocyte immunization. We present the result of 116 pregnancies followed at the Departamento de Tocoginecologia UNICAMP. Patients were thoroughly evaluated for causes of recurrent abortion mentioned in the literature (genetics, hormones, uterine abnormalities and infections), for autoimmune (antiphospholipid syndrome, abnormal autoantibodies) and for alloimmune causes (crossmatch by microlymphocytotoxicity and mixed lymphocyte culture). Patients who presented negative crossmatch and lower than 50% inhibition in mixed lymphocyte culture were treated with two concentrated intradermal paternal lymphocyte immunizations. Women were stimulated to attempt pregnancy with a positive crossmatch and higher than 50% inhibition in mixed lymphocyte culture. Women whose immune status did not change with this treatment were immunized again with paternal lymphocytes associated or not to a third party donor. We report that 81% of the women treated with this protocol had good pregnancy outcome.