Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2009;31(2):75-81
DOI 10.1590/S0100-72032009000200005
PURPOSE: to evaluate the factors leading to delays in obtaining definitive diagnosis of suspicious lesions for breast cancer. METHODS: a cross-sectional, observational study was carried out with 104 women attending a cancer hospital with a diagnosis or suspected diagnosis of breast cancer. A semistructured questionnaire on the patients' demographic, clinical characteristics and the use of services was applied.Variables were compared using t-Student test, Mann-Whitney test, Pearson's χ2 test or Fisher's exact test, as appropriate. In order to identify the variables associated with delays in breast cancer diagnosis, the Odds Ratio (OR) were calculated together with their respective 95% confidence intervals (95%CI) and a logistic regression model was constructed. RESULTS: age of patients was 54±12.6 years (mean±standard deviation). Most of the women were white (48.1%), married (63.5%), living in the city of Rio de Janeiro (57.7%) and poorly educated (60.6%). The median time between the first sign or symptom of the disease and first consultation was one month and the mean time between first consultation and confirmation of diagnosis was 6.5 months. In 51% of the women, diagnosis was late (stages II-IV). Symptomatic presentation and longer delay between symptom onset and the first evaluation and between symptom onset and the diagnosis were found to be significant factors (p<0.05) for delays in obtaining definitive diagnosis of suspicious lesions. CONCLUSIONS: the results of this study suggest that efforts must be made to reduce the time needed to get an appointment with a doctor and to confirm a diagnosis of suspicious lesions, as well as to educate physicians and the women themselves regarding the importance of breast symptoms and the value of prompt evaluation, diagnosis, and treatment.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2008;30(2):75-79
DOI 10.1590/S0100-72032008000200005
PURPOSE: the aim of this study is to evaluate the accuracy of mammography in the diagnosis of suspicious breast microcalcifications, using BI-RADS TM and Le Gal's classifications. METHODS: one hundred and thirty cases were selected with mammograms contain only microcalcifications of file and initially classified as suspicious (categories 4 and 5) without lesions clinical detectable and reclassified by two examiners, getting a consensus diagnosis. The biopsies were reviewed by two pathologists getting also a consensus diagnosis. Both, mammogram and histopathologic analysis were double blinded reviewed. Qui-square test, Fleiss-square statistic and EPI-INFO 6.0 were used in this study. RESULTS: the correlation between histopathological and mammographic analysis using BI-RADS TM and Le Gal classification showed the same sensitivity of 96.4%, specificity of 55.9 and 30.3%, positive predictive value (PPV) of 37.5 and 27.5%, and accuracy of 64.6 and 44.6% respectively. The PPV by BI-RADS TM categories was: category 2, 0%; category 3, 1.8%; category 4, 30.8%; and category 5, 60%. The PPV by Le Gal classification was: category 2, 3.1%; category 3, 18.1%; category 4, 26.4%;category 5, 66.7%, and non classified 5.2%. CONCLUSIONS: the results were better for the classification of BI-RADS™, but it did not get to reduce the ambiguity in assessment of breast microcalcifications.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(2):75-80
DOI 10.1590/S0100-72032006000200002
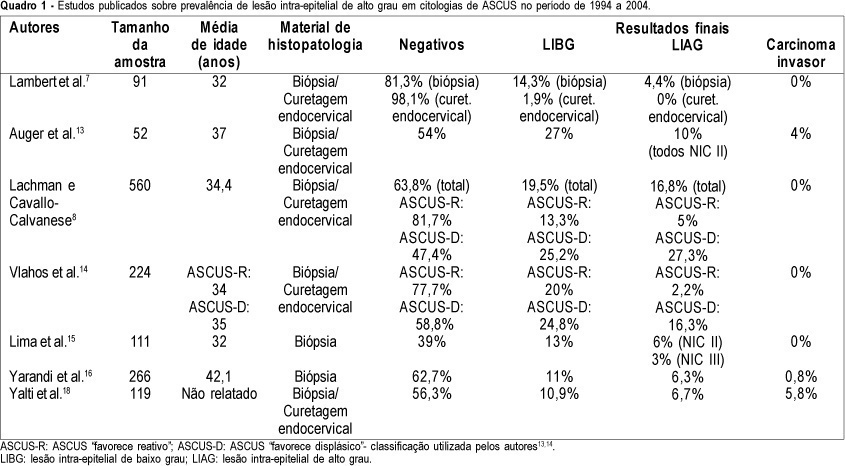
PURPOSE: to determine the prevalence of high-grade squamous intraepithelial lesions (HSIL) and cancer in women with cytological diagnosis of persistent ASCUS (atypical squamous cells of undetermined significance) for 6 months in the last 7 years. We also assessed if age could be a predictive factor for presence of HSIL/cancer in this group. METHODS: we included 215 cases of non-pregnant and HIV-seronegative women with cytological diagnosis of persistent ASCUS (unespecific) with at least 6 months of interval between smears. This cytological diagnosis was compared to histological diagnosis obtained by biopsy (large loop excision of the transformation zone) or cone biopsies, and considered negative when colposcopy was satisfactory without lesions or, when unsatisfactory, no lesion was detected after at least one cytological and colposcopic follow-up. RESULTS: among the 215 cases, 49.3% had negative results (CI 95%: 42.6-55.9). The prevalence of histological confirmed low-grade squamous intraepithelial lesion was 38.6% (CI 95%: 32.1- 45.1) and HSIL was 10.7% (CI 95%: 6.5-14.8). Cases of cancer were found in 1.4% of patients (CI 95%: 0-2.9). We could not find a significant difference between the prevalence of HSIL/cancer according to age group using the cutoff point of 35 years. CONCLUSION: HSIL/cancer prevalence observed in this study has shown the risk of finding this kind of lesions in about 12% of women assisted in our public health system with two cytological diagnosis of ASCUS. A higher probability of HSIL/cancer in the different age groups was not found but this result was limited by our small sample size.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(12):750-758
DOI 10.1590/S0100-72032005001200008
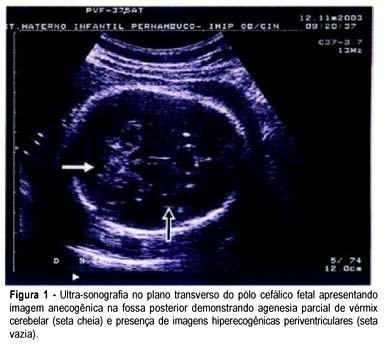
Congenital cytomegalovirus infection is an important clinical entity, due to its sonographic symptomatology. In Brazil, in utero diagnosis is not accomplished despite the improvements in diagnostic methods. We report a congenital infection including: splenomegaly and hepatomegaly, hypoplasia of the cerebellar vermis, intracranial calcifications, hyperechoic kidneys, hyperechoic bowel, cardiomegaly, lung hypoplasia, ascites, and pericardial effusion. Fetal magnetic resonance imaging confirmed the sonographic findings. Amniocentesis was performed for cytomegalovirus PCR in amniotic fluid, which confirmed fetal infection. Fetal loss occurred in the 31st week of pregnancy. Necropsy studies confirmed the sonographic findings. The diagnostic methods have been useful to confirm congenital cytomegalovirus infection and to establish fetal outcome.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(10):752-753
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(10):752-752
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2020;42(11):752-758
To identify whether the effects of thyroid disease during pregnancy and lactation affect the nutritional composition of human milk.
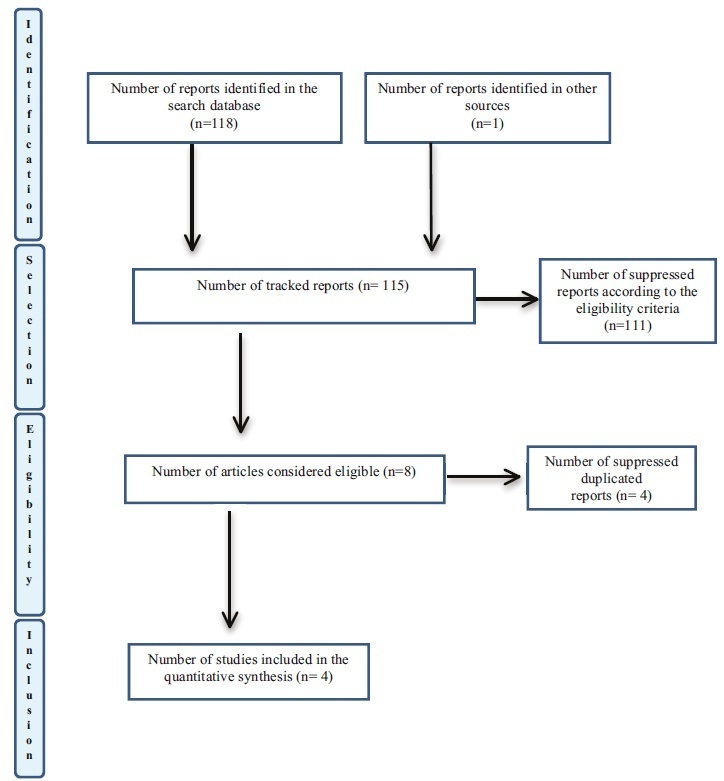
Systematic review of the scientific literature using the Medical Literature Analysis and Retrieval System Online/MedLine databases to evaluate the association of thyroid diseases during pregnancy and lactation with the nutritional composition of human milk. There was no delimitation by period or by language, and the searches were completed in March 2019. The following descriptors were applied: human milk AND thyroid AND composition, using the preferred reporting items for systematic reviews and meta-analyses (PRISMA) protocol for data search, selection, and extraction. The flowchart proposed for bibliographic search resulted in 12 articles and, of these, four were selected.
The articles elected for this review were published between 1976 and 2018. Two studies found significant differences in the nutritional composition of mothers' milk with hypothyroidism or overweight compared with the milk of those without hypothyroidism. Studies have shown that the presence of the disease led to changes in the nutritional composition of human milk, especially a higher concentration of human milk fat.
It is extremely important that these women have continuous nutritional follow-up to minimize the impact of these morbidities on the nutritional composition of human milk.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(10):753-753