Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2017;39(12):653-658
To identify the prevalence of pyelonephritis during pregnancy and to analyze the clinical and laboratorial aspects, perinatal results and complications.
A transversal study of 203 pregnant women who had pyelonephritis during pregnancy and whose labor took place between 2010 and 2016 at a hospital in the state of Santa Catarina, Brazil. The analysis was based on medical records as well as on the hospital’s database. Clinical and laboratory conditions, antibiotics, bacterial resistance, perinatal outcomes and complications were all taken into account. The data was compared using the Mann-Whitney test and the Chi-square test.
A prevalence of 1.97% with pyelonephritis was evidenced, with most patients having it during the second trimester of gestation. The bacteriamost commonly found in the urine cultures was Escherichia coli, in 76.6% of cases, followed by Klebsiella pneumoniae (8.7%). Ceftriaxone had the lowest bacterial resistance (only 3.5% of the cases). On the other hand, ampicillin and cephalothin presented higher bacterial resistance, 52% and 36.2%, respectively. The risk of very premature delivery was more than 50% higher in patients with pyelonephritis.
Ampicillin and first-generation cephalosporins are associated with a higher bacterial resistance while ceftriaxone proved to have a high efficacy for the treatment of pyelonephritis due to low bacterial resistance. Patients with pyelonephritis showed a higher risk for very premature delivery (< 32 weeks). In this casuistry, there were no others significant differences in the overall perinatal outcomes when compared with the routine service series.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2023;45(11):654-660
To evaluate the continuation rates of the 52-mg levonorgestrel-releasing intrauterine system (LNG-IUS) during the first 5 years of use, reasons for its discontinuation, bleeding patterns, and new contraceptive choice after the 5th year, in adolescents and young women.
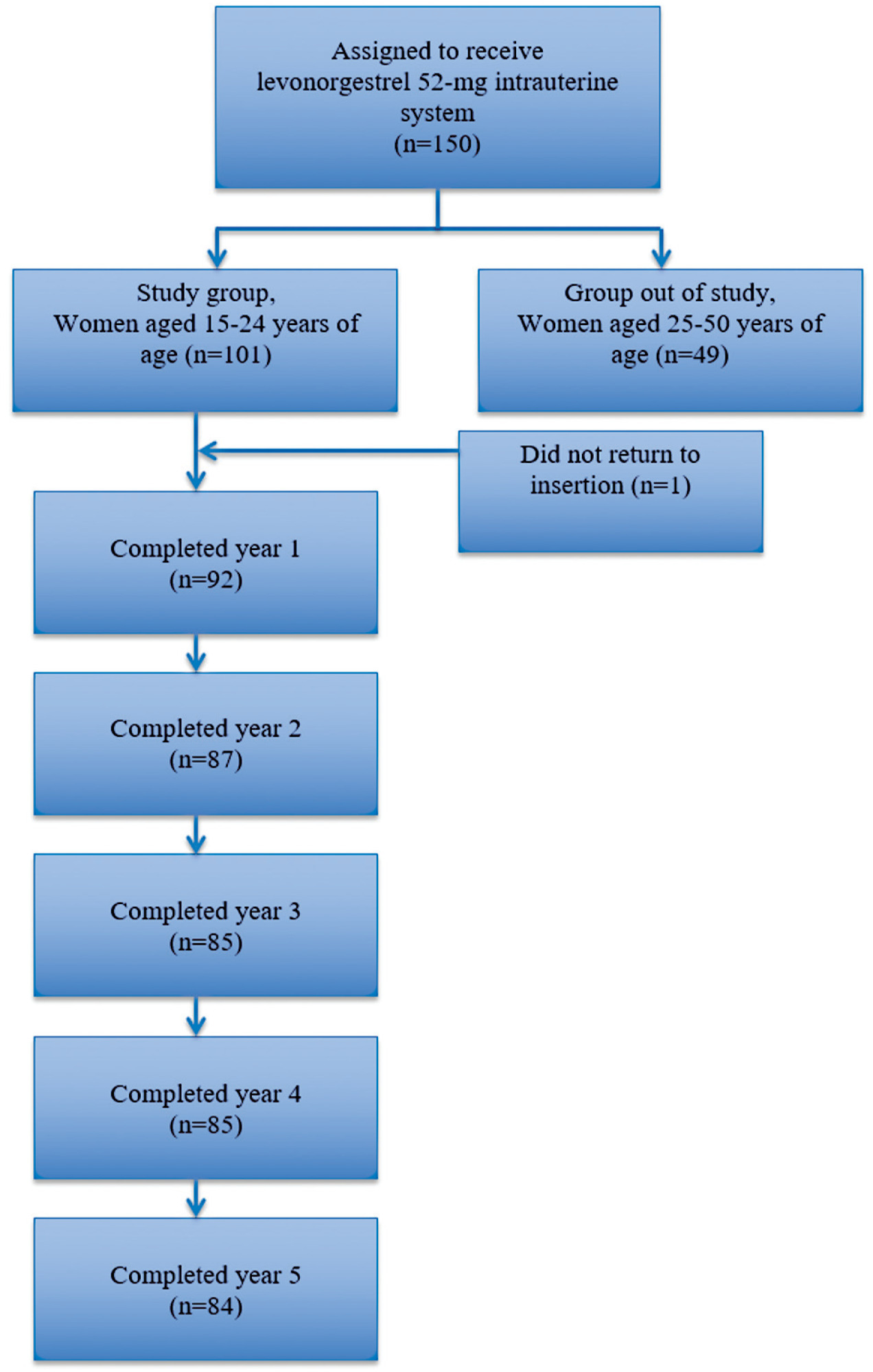
The present study was a 5-year prospective cohort conducted in a Family Planning Service of a tertiary hospital in Brazil. We selected 100 healthy women between 15 and 24 years old who used 52-mg LNG-IUS for contraception. The clinical follow-up of these women took place from June 2017 to December 2022. The study evaluated the continuation rates of the method, reasons for its discontinuation, bleeding patterns, and new contraceptive choice after the 5th year. Continuous data were reported as mean ± standard deviation (SD) and range (minimum-maximum). Categorical variables were described as percentages.
The continuation rates of LNG-IUS were 89.1% (82/92), 82.9% (72/87), 75.3% (64/85), 70.5% (60/85), and 64.2% (54/84) in the 1st, 2nd, 3rd, 4th, and 5th years of use, respectively. The main reason for discontinuation was acne (11/30). Amenorrhea rates were 50, 54.1, 39, 35.7, and 51.8% at 12, 24, 36, 48, and 60 months, respectively. All patients who completed the study and needed contraception after the 5th year opted for long-acting contraceptive methods (LARC).
The LNG-IUS showed high continuation rates in adolescents and young women in the first 5 years of use. Most patients who completed the study chose a LARC method after the 5th year.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2022;44(7):654-659
Urodynamic studies (UDSs) are a set of tests that assess the storage and emptying of urine, and they are widely used by gynecologists and urologists in the management of urinary incontinence (UI), despite the discussion about its indications. The objectives of the present study were to verify whether UDSs are routinely used in the conservative and surgical approaches to female UI, their other clinical indications, and to compare the responses of Brazilian gynecologists and urologists.
The present is an opinion survey applied from August 2020 to January 2021 through a semistructured questionnaire about the clinical practice sent by e-mail to all participants. The responses were compared through statistical analyses.
Of the 329 participants, 238 were gynecologists (72.3%) and 91, urologists (27.7%). Most gynecologists (73.5%) and urologists (86.6%) do not request UDSs before the conservative treatment of UI; but UDSs are indicated in the preoperative period of anti-incontinence surgeries. Most participants request UDSs in the initial approach to overactive bladder (gynecologists: 88.2%; urologists: 96.7%), and the urologist has greater chance to request this study (odds ratio [OR] = 3.9). For most participants, it is necessary to request uroculture before the UDSs.
Most Brazilian gynecologists and urologists who participated in the present study do not request UDSs before the conservative treatment of UI, according to national and internacional guidelines, and often request it before the surgical treatment for female UI. The indication of this exam in the initial approach of idiopathic overactive bladder should be reviewed by the participants.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(10):654-655
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(10):654-655
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2019;41(11):654-659
To evaluate the outcomes of cases of prenatally-diagnosed congenital pulmonary airway malformation (CPAM).
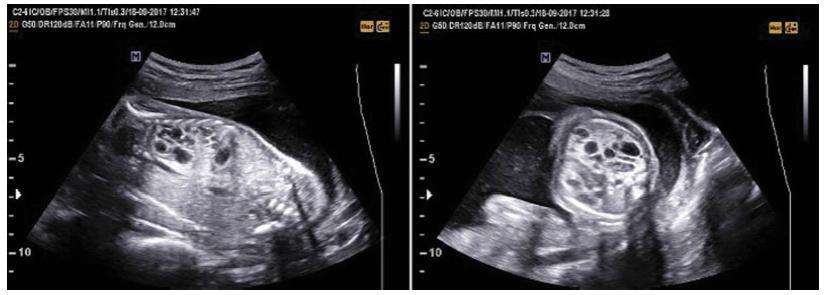
We retrospectively evaluated cases of prenatally-diagnosed CPAM between 2004 and 2018. Ultrasonographic features such as visualization of a fetal lung mass and heterogeneous pulmonary parenchyma were used for CPAM diagnosis. Prenatal and postnatal findings were compared in terms of accuracy regarding the CPAM diagnosis.
The sample consisted of 27 cases. There were four cases in which the patients opted for the termination of pregnancy due to the severity of the lesion. A total of 23 neonates were delivered, and CPAM was confirmed in 15 cases. Themedian gestational age at delivery was 37 weeks (28-40 weeks) and the mean birth weight was 2,776 g. There were two neonatal deaths, one due to pneumothorax, and the other due to hypoplastic left heart syndrome (HLHS). A total of five patients with respiratory problems were operated in the postpartum period. There were eight misdiagnosis: bronchopulmonary sequestration (five cases), congenital lobar emphysema (two cases), and congenital diaphragm hernia (one case).
A precise postnatal diagnosis is very important to organize the proper management of the pregnancies with fetuses with CPAM. The positive predictive value of the prenatal diagnosis of CPAM via ultrasonography is of 70.3%. The differential diagnosis of CPAM may be prolonged to the postpartum period in some cases.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2003;25(9):655-659
DOI 10.1590/S0100-72032003000900006
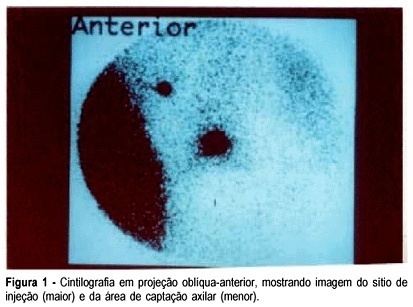
PURPOSE: to assess the simultaneous approach of radioguided occult lesion localization and sentinel lymph node biopsy in women with breast cancer. METHOD: forty-five patients with nonpalpable breast cancer were enrolled in a prospective study. The employed radiocolloid was 99mTc-labelled dextran. The injection was performed peritumorally under sonographic or stereotactic guidance using a 18 gauge needle. Lymphoscintigraph images for the visualization of both the site of injection and sentinel lymph node were obtained in a conventional gamma-camera, with the ipsilateral arm positioned in a 90º angle. Excision biopsy of the tumor and sentinel lymph node were performed with a gamma-detecting probe. RESULTS: the procedure was always successful in permitting the localization of occult breast lesions. It was necessary to enlarge surgical margins in five cases. Concerning the sentinel lymph node we achieved localization in 93% of the cases. No complications were observed. CONCLUSION: the results seems to demonstrate that a combined radioguided occult lesion localization and sentinel lymph node biopsy using the same radiopharmaceutical represents a useful and practicable strategy in the management of early breast cancer.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2002;24(10):655-661
DOI 10.1590/S0100-72032002001000004
PURPOSE: to evaluate the effects of antenatal corticosteroid treatment on the incidence of respiratory distress syndrome (RDS), neonatal morbidities, and mortality in preterm babies assisted at IMIP, a teaching hospital in Brazil. METHODS: this was an observational, analytical, cohort study which included 155 newborns from women who delivered prematurely. The study was conducted between February and November 2001 and included 78 women in the corticosteroid-treated group and 77 in the nontreated group. The study design included the incidence of RDS, assessment of morbidities related to prematurity and tabulation of neonatal mortality. The risk ratio and its 95% confidence interval were determined for estimation of the relative risk for RDS and neonatal outcome (dependent variables) according to antenatal corticoid therapy administration (independent variable). RESULTS: corticosteroid treatment was administered to 50.3% of the patients (64% of the women received the full treatment course, while 36% of the same group received a partial course of treatment). The incidence of RDS was significantly lower in the corticosteroid treated group (37.2%) compared with the nontreated group (63.6%). There was no observable decrease in the risk for morbidities associated with prematurity. There was a decrease in mortality and in the frequency of supplemental oxygen therapy in the corticosteroid group (37%). On multiple logical regression analysis, there was a 72% reduction in the risk for RDS in the corticosteroid group, and approximately a seven times greater risk for RDS in babies of gestational age below 32 weeks. CONCLUSIONS: a favorable impact of antenatal corticosteroid administration was observed, with significant reduction of the risk for RDS in patients with gestational age between 26 and 35 weeks. Although no effect on the other morbidities was observed, this can be explained by the small size of the sample.