Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(2):65-70
DOI 10.1590/S0100-72032000000200002
Purpose: to evaluate conization by the loop electrosurgical excision procedure (LEEP) for the diagnosis and treatment of cervical intraepithelial neoplasms (CIN), the importance of the margins and follow-up of these women. Methods: 95 women who underwent conization by LEEP for CIN and microinvasive carcinoma from January 1996 to December 1997 were evaluated. For statistical analysis, we used the kappa agreement coefficient and the tendency test of Cochran Armitage. Results: among 63 cases who underwent colposcopically directed biopsy before the conization, the cone presented the same grade of lesion in 20 and no residual disease in 8. The cone lesion presented a higher grade in 24 cases and one of them was a microinvasive carcinoma. Among the 25 women who underwent the cone biopsy with a previous biopsy suggestive of cervicitis or CIN 1, 56% had CIN 2 or 3 in the cone. Among the 32 women without previous biopsy, 15 had CIN 2 or 3, and four had microinvasive carcinoma in the cone. Regarding the margins of the cone, 25 cases presented some grade of CIN in the endocervical margins and 2/10 who underwent a second procedure presented residual disease on histological analysis. Among the 70 women with free cone margins, 2/4 who underwent a second procedure had residual disease on histological analysis. Conclusion: conization by LEEP without previous directed biopsy depends on the experience of the colposcopist. The second resection after LEEP for the diagnosis and treatment of CIN depends not only on the presence of disease in the cone margins but also on the follow-up. A second histological analysis is recommended in cases with microinvasive carcinoma and glandular lesion and affected margins.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(10):650-651
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(11):650-655
DOI 10.1590/S0100-72032005001100003
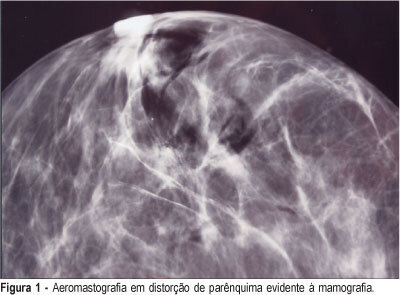
PURPOSE: to asses the efficiency of the radioguided localization and removal of occult breast lesions using radiopharmaceuticals injected directly into the lesions or close to them with posterior air injection as a radiological control. METHODS: twenty-nine consecutive patients with thirty-two occult breast lesions detected mammographically or by ultrasound, and categorized 3, 4 and 5 BI-RADS®, were included in this observational study with results expressed in percentages. The radiopharmaceutical used was human serum albumin labeled with 99mTc-HSA injected inside or close to the lesion using mammographic or ultrasonographic guidance. The injection of the radiopharmaceutical was followed immediately by air injection through the needle used for stereotaxis as a radiological control of the radiopharmaceutical placement. The excision biopsy was carried out with the aid of a hand-held gamma-detecting probe and the entire removal of the lesion was verified by X-ray of the surgical specimens or by intraoperative frozen section examination. RESULTS: breast cancer was found in 10.0% (1/10) of the 3 BI-RADS® lesions, in 31.5% (6/19) of the 4 BI-RADS® and in 66.6% (2/3) of the 5 BI-RADS®. The radiotracer was correctly positioned in 96.8% of the specimens (31/32) allowing the removal of also 96.8% of the studied non-palpable breast lesions. To show the entire removal, X-ray was used in 23 cases (71.8%), intraoperative frozen section study in 21.8% (7/32) and both methods in 6.2% (2/32). CONCLUSIONS: radioguided surgery showed to be an important tool in the removal of non-palpable breast lesions, as a simple, fast and feasible method that can be implemented in the clinical routine of these patients.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(10):652-653
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2018;40(10):652-653
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2006;28(11):652-657
DOI 10.1590/S0100-72032006001100004
PURPOSE: to determine if the previous fertility history can predict current fertility status of a patient examined for couple’s infertility. METHODS: retrospective study involving semen analyses from 183 consecutive subfertile patients evaluated from September 2002 to March 2004. We excluded those patients who had undergone radio or chemotherapy, orchiectomy or vasectomy. Mean values of all analyses were used for patients with multiple semen analysis. Patients with more than 20x10(6) sperm/mL, motility higher than 50% and with normal strict sperm morphology higher than 14% were considered normal. Patients were divided into two groups, according to the fertility status: primary infertility (118 patients) and secondary infertility (65 patients). Data were analyzed according to the chi2 test and the Student t-test. RESULTS: no differences were detected in the mean age between patients with primary infertility, 37.3±6.3, and secondary infertility, 38.1±5.9; p=0.08. In the group of patients with primary infertility, 51.9% (61 patients) had a normal sperm concentration, 70.3% (83 patients) had normal sperm motility and 26.3% (31 patients) had normal sperm morphology. In the group of patients with secondary infertility, 53.8% (35 patients) had normal sperm concentration, 75.4% (49 patients) had normal sperm motility and 32.3% (21 patients) had normal sperm morphology. No significant differences were detected in sperm concentration (21.3x10(6)/mL versus 23.1x10(6)/mL; p=0.07), motility (45.2 versus 48.1%; p=0.08) and morphology (6.1 versus 6.4%; p=0.09) between groups of patients with primary and secondary infertility. CONCLUSIONS: semen analysis should be requested even in cases of prior male fertility. Physicians should not presume a patient to have a normal semen analysis based on his previous history of initiating a pregnancy.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2000;22(10):653-656
DOI 10.1590/S0100-72032000001000009
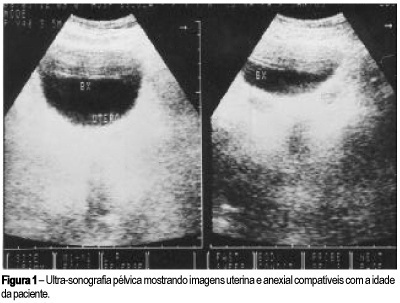
Chronic appendicitis might simulate several diseases, making clinical management difficult. We report the case of a 9-year-old girl with an abdominal pain for 13 months. Ultrasound and tomography showed an expansive mass in the lower abdomen. It was extremely difficult to establish the diagnosis because the symptoms, laboratory results and images were inconclusive. The definitive diagnosis occurred only after laparotomy. We discuss in the present article several differential diagnoses for chronic appendicitis, mainly gynecological malformations, endometriosis, neoplasias and pseudotumors.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2001;23(10):653-657
DOI 10.1590/S0100-72032001001000007
Purpose: to verify if there is an association between the mean blood velocity in the descending thoracic aorta and fetal anemia diagnosis. Methods: this is a prospective, cross-sectional study in which the mean blood velocities in the fetal aorta, in 66 fetuses at risk for severe anemia due to severe Rh immunization, and cord blood hemoglobin levels were analyzed comparatively. The hemoglobin level was obtained by cordocentesis if an intravascular transfusion was performed for severe anemia, however, if the fetus received an intrauterine transfusion by the intraperitoneal route or if the fetus did not receive a transfusion at all, hemoglobin level was measured at the time of pregnancy termination by umbilical cord puncture. The authors made a statistical association between the mean blood velocity in fetal descending thoracic aorta and the diagnosis of fetal anemia. The c² test was used for statistical analysis and a p value <0,05 was used to indicate significance. Results: there was a significant and indirect association between the mean blood velocity in the descending thoracic aorta and the detection of fetal anemia. The mean blood velocity in fetal thoracic aorta had a sensitivity of 47.4% for the diagnosis of moderate fetal anemia (Hg<10.0 g/dL), with a p value <0.01 by the Fisher exact test, and a sensitivity of 54.5% for severe Rh isoimmunization (Hg<7.0 g/dL), with a p value =0.01. Conclusion: this study revealed a significant indirect correlation between mean blood velocity in the descending thoracic aorta and the detection of fetal anemia due to Rh isoimmunization.