Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(6):347-352
DOI 10.1590/S0100-72032005000600009
PURPOSE: to assess the interference of two vaginal lubricants (vaseline and silicone) in the interpretation of cervical oncotic cytology. METHODS: a prospective research on one hundred women from August to October 2003. The women were divided into two groups of 50 patients each, according to the type of lubricant used. Two smears were obtained from every patient: the first specimen soon after the introduction of non-lubricated speculum and the second after the use of lubricated speculum with vaseline (Group V) or silicone (Group S). The samples were analyzed by two cytotechnicians, who were unaware of the origin of the smears. RESULTS: among the 100 pairs of slides, 8 results were partially different. The reasons for the differences were not directly related to the use of lubricant and did not interfere with the cytologic findings. The number of discordant results was 6 in Group S and 2 in Group V, without a statistically significant difference (p=0.269). The number of satisfactory and satisfactory but limited results was statistically similar regarding the use or not of lubricant: Group S: 46 satisfactory slides and 4 satisfactory but limited slides (p=0.001 and kappa=0.802) and Group V: 48 satisfactory and 2 satisfactory but limited slides (p=0.001 and kappa=0.953). There were no unsatisfactory results. No artefacts were found in slides obtained with lubricated speculum. CONCLUSION: the use of lubricated speculum with vaseline or silicone does not affect cervical oncotic cytology outcome.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(6):353-356
DOI 10.1590/S0100-72032005000600010
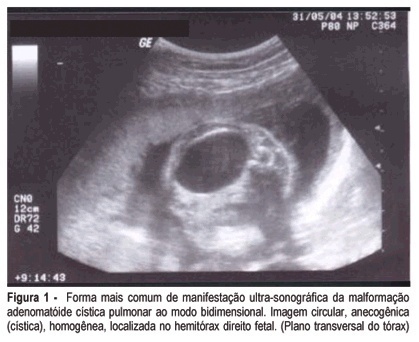
Fetal cystic adenomatoid malformation is a pulmonary developmental anomaly arising from an overgrowth of the terminal respiratory bronchioles. This is such a rare malformation, that is not always thought of as a diagnostic possibility. We present a case of pulmonary cystic adenomatoid malformation and emphasize the importance of early diagnosis and therapeutic possibilities. We also present its evolution after prenatal placement of a catheter for continuous drainage.
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(6):357-365
DOI 10.1590/S0100-72032005000600011
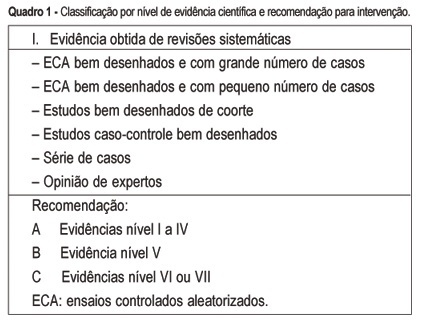
The multiple factors involved in maternal complications and maternal mortality make the task of their long-term control difficult and time-consuming. Professional care for pregnant women and/or those in labor certainly represents a key point for obtaining good outcomes, either maternal or perinatal. From the starting point that an adequate professional medical care for delivery has the capacity of decreasing the occurrence of complications associated with maternal morbidity and mortality, the evidence regarding some interventions included in this care is summarily presented. The evidence derived from studies performed with a strong methodological and scientific approach, mainly randomized controlled trials, on interventions to reduce complications and maternal mortality. These main interventions basically refer to: institutional care to is focused delivery, skilled professional care, use of traditional birth attendants in some contexts, use of appropriate technologies including partograph, place of birth, position for delivery, use of episiotomy, type of delivery, use of oxytocin during the active phase of labor, performance of push efforts during the second stage, active management of the third stage, and prophylaxis for post-partum hemorrhage. Although the effect of avoiding maternal death is difficult to be evaluated due to its low frequency, its rational and standardized use, through manuals and guidelines for intervention care, has a positive effect on the quality of care for childbirth. This is part of the human and technical context of the right that every woman has to the best possible care in this so special moment of her life.

Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(6):366-366
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(6):366-366
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(6):367-367
Summary
Revista Brasileira de Ginecologia e Obstetrícia. 2005;27(6):367-367